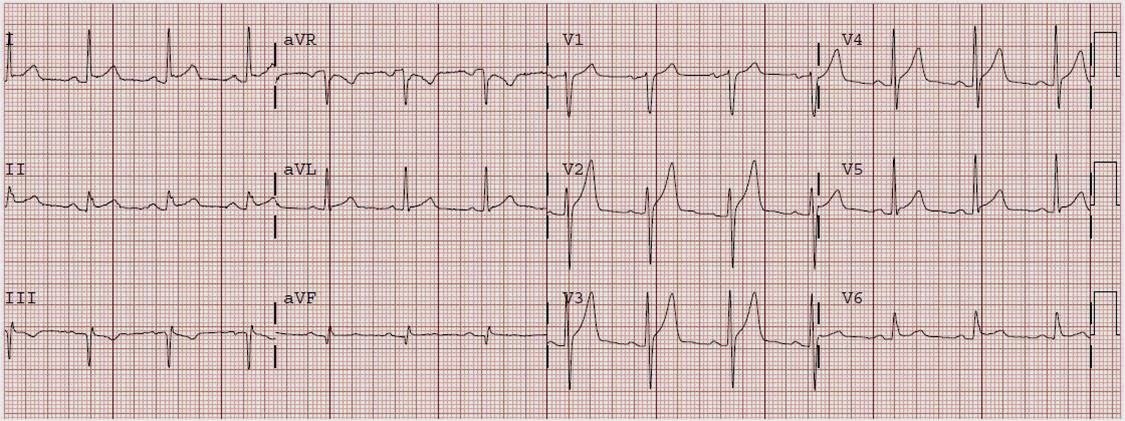
A 45-year-old male was in his usual state of health until three hours prior to arrival, when he developed left-sided chest pressure with radiation to the neck while walking. His pre-hospital ECG is identical to the first emergency department ECG shown in Figure 1. Based on this, the paramedics activated the cath lab, administered nitroglycerin, and the pain resolved.
This is when the Early Repolarization vs LAD Occlusion Equation can be applied – STE60V3 is 4 mm, QTc is 416ms, and RA-V4 is 15mm. Plugging these values in yields 23.753. Being > 23.4, the equation points to STEMI. The specificity of the rule is not perfect, but a value above 23.4 should at least prompt you to aggressively evaluate the patient.
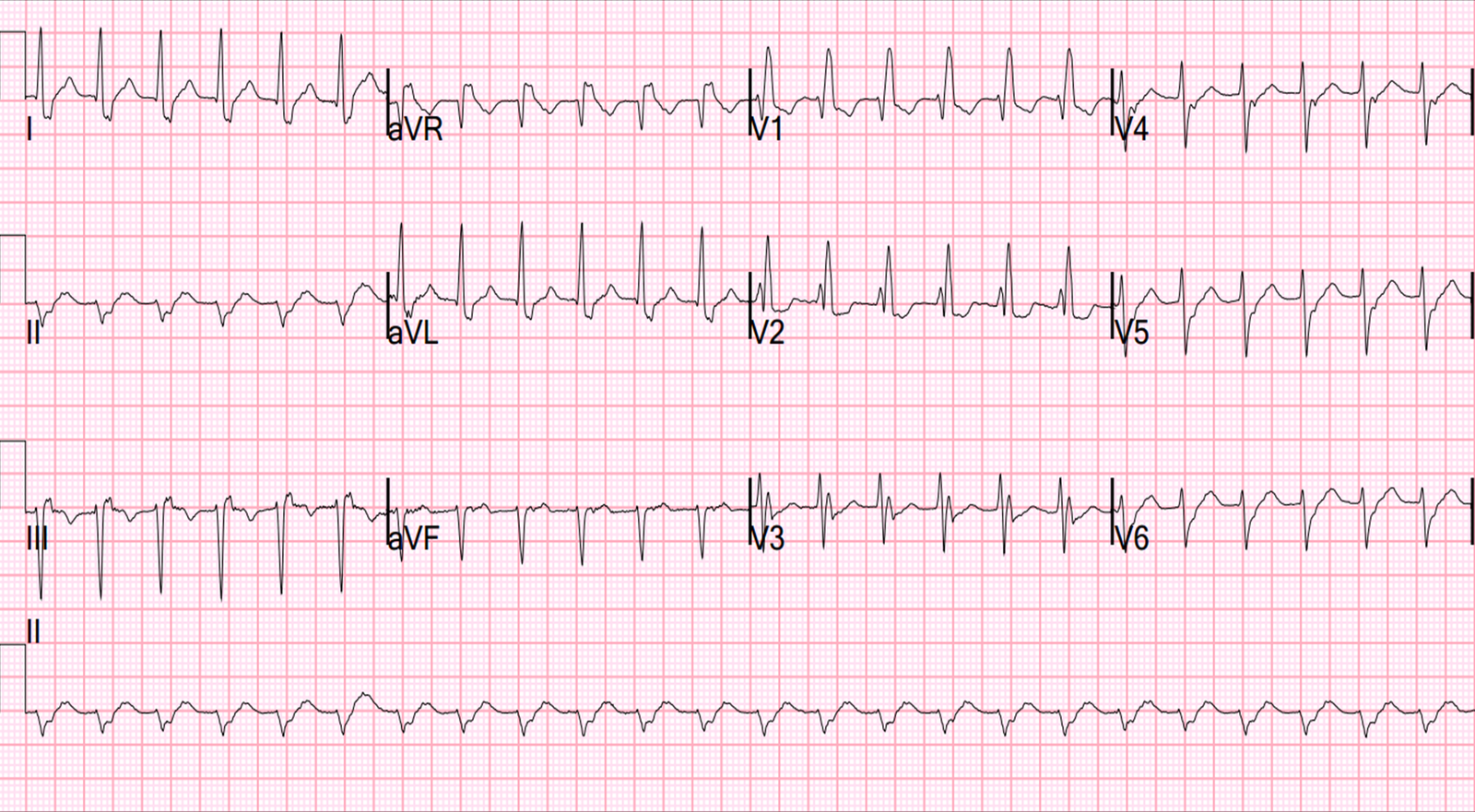
As for the patient’s clinical course, his chest pressure resolved. A bedside emergency department echocardiogram (not a formal echo) reportedly showed no wall motion abnormality. The equation was not used. The cath lab was de-activated. A repeat ECG showed less ST-elevation:
An application of the Early Repolarization vs LAD Occlusion Equation has equivocal results, depending on whether the STE60V3 is measured at 1.5 or 2.0 mm. Nevertheless, the change shows that the previous ECG was indeed due to acute coronary syndrome (ACS).
Remember – not all ACS has a positive troponin! When negative, it is – of course – called “unstable angina.” It usually presents with a normal or nonspecific ECG, with ST-depression, or T-wave inversion – but unstable angina may also present with transient ST-segment elevation. Perhaps more disgruntling, transient ST-elevation does not always result in a positive troponin. The ischemia may resolve so quickly that there is both no wall motion abnormality and the troponin is negative!
With the advent of high-sensitivity troponin in the future, perhaps such cases will become more rare. But this increased sensitivity may come at the expense of worse specificity, or more false positive troponins.
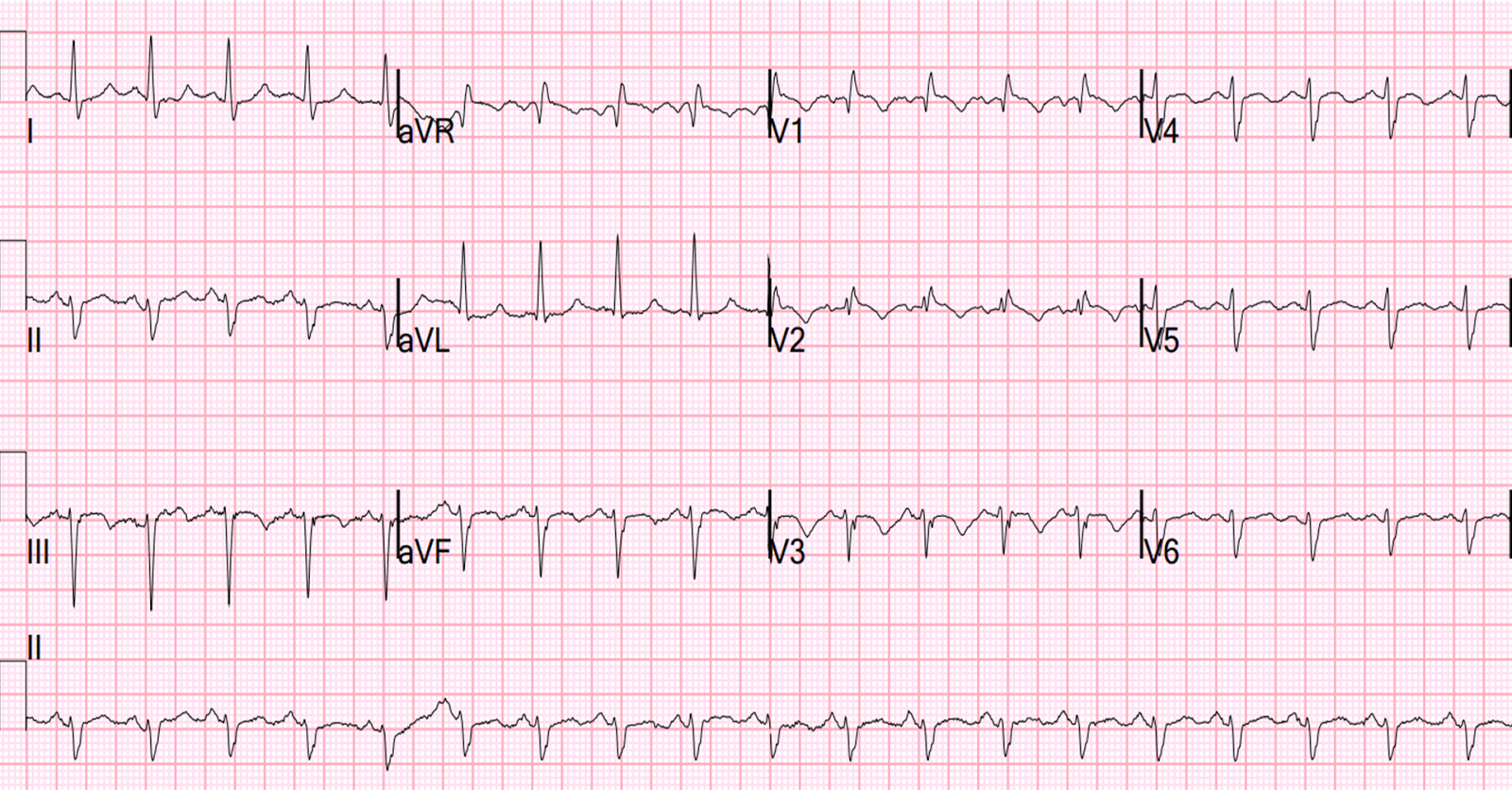
The patient ruled out for acute MI with serial troponins remaining < 0.04 ng/ml (using a sensitive troponin assay). And so the patient was discharged. Yet 13 days later, he again presented with chest pain that again resolved. Another ECG was done after resolution of pain, as seen in Figure 3.
This time troponin was positive, and the patient underwent coronary angiography, which showed severe subtotal left anterior descending artery disease and 70% left main disease. He underwent coronary artery bypass surgery.
Lessons
1. This case illustrates the importance of paying close attention to the ECG and its evolution. The initial ECG is extremely difficult to differentiate from early repol, though the formula did so handily. But the diagnosis is much easier if one pays attention to the change on the subsequent ECG. With the formula applied, this patient’s ACS could’ve have been diagnosed earlier. He could easily have died in spite of a negative troponin.
2. Serial negative troponins do not rule out ACS. One still must pay attention to the ECG.
3. If a formal echo had been done the next day, it most likely would have been normal as well: stunning in such cases resolves quickly. See this case. And this case.