Written by Jesse McLaren, edits by Smith
A 75 year old without cardiac history presented to the emergency department with 3 hours of acute chest pain, which radiated to the jaw and bilateral shoulders. The question “to cath or not to cath” was answered with 5 common reasons:
- there was no STEMI criteria on serial ECGs
- there was no reciprocal change
- the first troponin was normal
- second troponin not very high
- absence of evolution to ST elevation
- the pain improved with nitro
Go through the case and at each step ask the question: to cath or not to cath?
Here’s the triage ECG and repeat 30 minutes later:
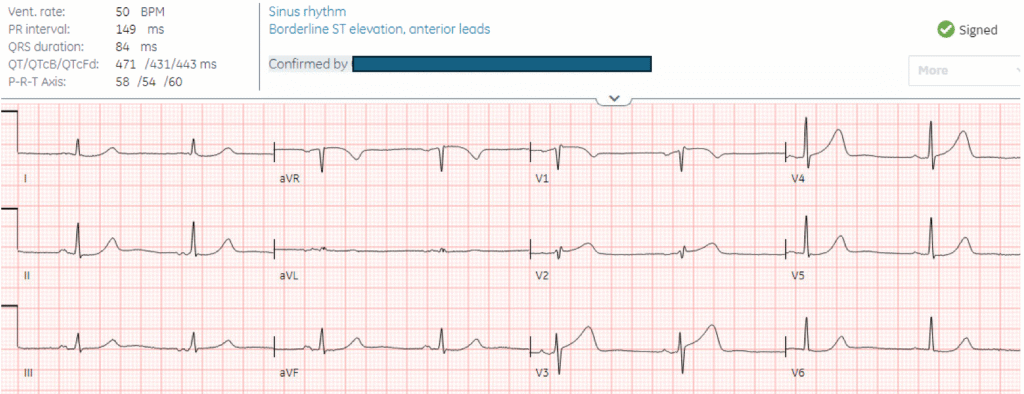
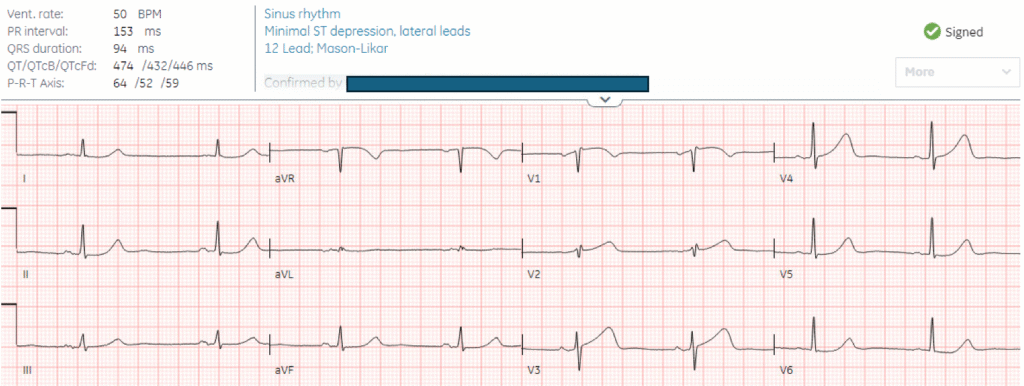
What do you think?
There’s sinus bradycardia, normal conduction, normal axis, normal R wave progression, and voltages. The minimal ST elevation in the anterior leads is normal. On the other hand, the T waves in V2-4 are wide based, bulky, and large relative to their QRS (and compared with the other leads, where the T waves have a small area under the curve). On repeat ECG the ST segment is straightening in V3, and there’s ST depression in V6 (identified on the final read as ‘minimal ST depression, lateral leads’).
1. No STEMI criteria? We know from the systematic review and meta-analysis by de Alencar et al that this is only 43% sensitive for Occlusion MI. The 2022 ACC expert consensus has added hyperacute T waves to the list of “STEMI equivalents”.
2. No reciprocal change? The “PAILS” mnemonic teaches that anterior ST elevation produces inferior reciprocal ST depression, but these leads are in different planes and are not reciprocal to each other. In the horizontal plane of the precordial leads, anterior and posterior leads are reciprocal to each other, while V1 is reciprocal to V6. In the frontal plane of the limb leads, the inferior and high lateral leads are reciprocal to each other. LAD occlusion only produces inferior ST depression if this is reciprocal to high lateral ST elevation (from occlusion proximal to the first diagonal) which is not present here. On the other hand there is ST depression in V6 which is reciprocal to V1 (precordial swirl), indicating occlusion proximal to the septal branch. Furthermore, there is a tiny bit of reciprocal ST depression in II and aVF, clearly abnormal
So based on STEMI criteria and “no reciprocal change”, the cath lab was not activated.
A Troponin was sent. Was this the correct decision?
I sent it to Dr. Smith without any information, and he replied “I’d have to say it is LAD Occlusion.” That is to say, cath lab now.
In addition, based on expert-trained AI interpretation, the patient presenting with classic symptoms of ACS has an ECG diagnostic of OMI. Here’s the Queen of Hearts interpretation of the first ECG, highlighting the hyperacute T waves and subtle precordial swirl:
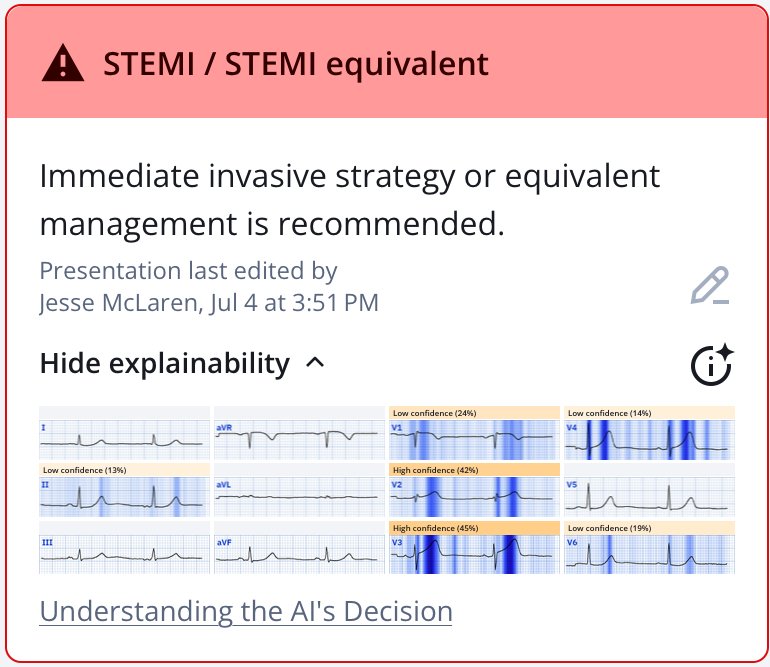
New PMcardio for Individuals App 3.0 now includes the latest Queen of Hearts model and AI explainability (blue heatmaps)! Download now for iOS or Android. https://www.powerfulmedical.com/pmcardio-individuals/ (Drs. Smith and Meyers trained the AI Model and are shareholders in Powerful Medical.)
Case continued
The first troponin came back at 8 ng/L (normal <16 in females and <26 in males), appearing to confirm the decision not to activate the cath lab. What do you think?
3. First troponin normal. Troponin is a rear view mirror which only shows damage in the past, not which has just happened or which is ongoing. In the context of acute symptoms the first troponin is unreliable to detect MI: it is <99th percentile in 14% of patients with STEMI, including almost a quarter of those presenting within two hours. In fact, even an hs-cTnI level as high as 50 ng/L (with URL of 34 ng/L) only has a PPV of 25% as such positive but low levels are present in many Non-AMI conditions. And the troponin doesn’t indicate the current state of the artery (open vs closed), but we can tell the current state of affairs from symptoms (ongoing chest pain) and ECG (hyperacute T waves). Moreover, while you are waiting for troponin, myocardium is dying. Thus, you should use the ECG, not troponin, to make the emergent cath lab decision.
4. 2nd Troponin not high enough. The chest pain continued and a repeat troponin 2 hours later increased to 46 ng/L. This is a delta of 38 ng/L, and has a specificity of 97% for Acute MI (whether Type I or Type 2). The patient was given nitro and a repeat ECG was done, which was also “STEMI negative” so the patient was referred to cardiology as a “non-STEMI”.
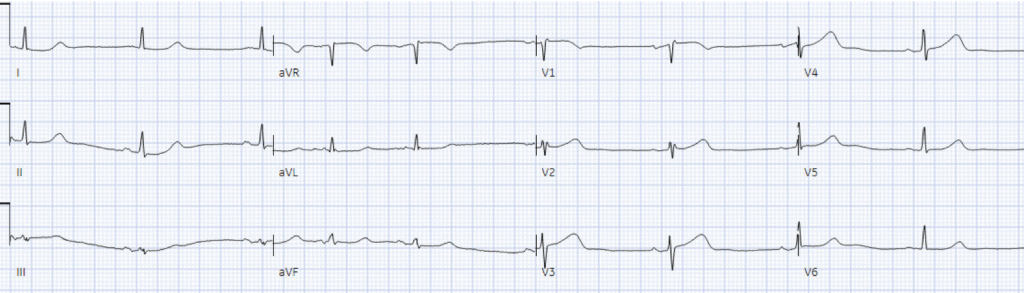
Cardiology saw the patient 5 hours after arrival, and documented incorrectly that there were no dynamic ECG changes, and that nitro had improved the pain from 7/10 to 3/10, so the patient was admitted as “Non-STEMI”. What do you think?
5. Absence of evolution to ST Elevation. There is still no STEMI criteria, and hyperacute T waves have not progressed to STEMI. But contrary to popular opinion, hyperacute T waves do not always progress to STE. On the other hand, the hyperacute T wave have partially deflated and the ST depression in V6 has resolved – so there have been dynamic changes. Smith and Meyers have a paper pending publication that shows that, of 53 TIMI-0 LAD cases, only 33 met STEMI criteria and NONE of the 20 without STE developed STEMI criteria on subsequent ECGs.
Here’s the comparison of the precordial leads for the first 3 ECGs, showing the inflation and partial deflation of hyperacute T waves, and transient STD in V6:
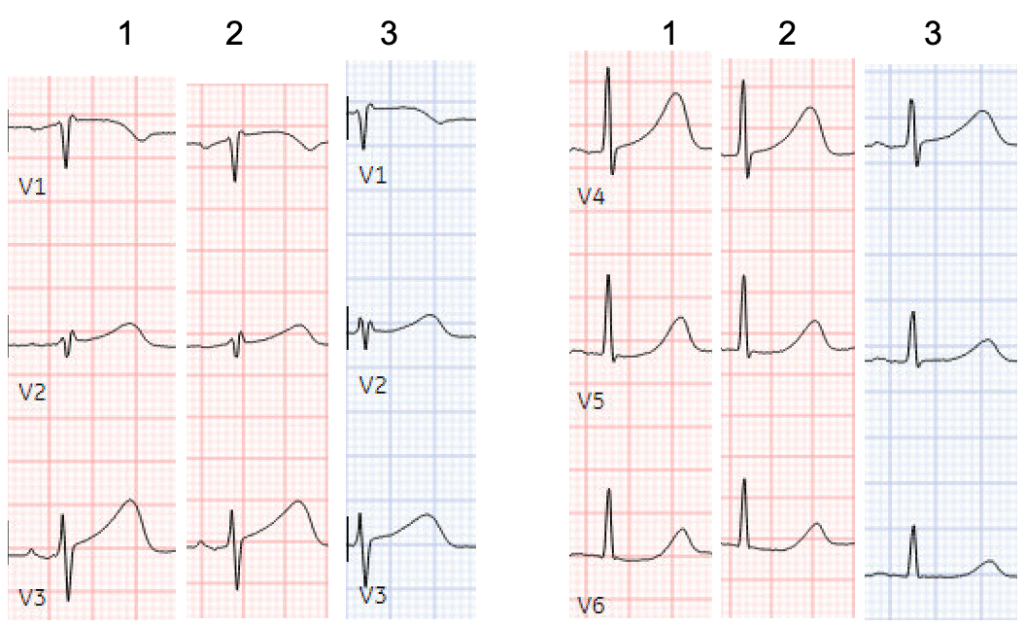
Even with this improvement, and without the prior to compare, the Queen of Hearts still identifies hyperacute T waves:
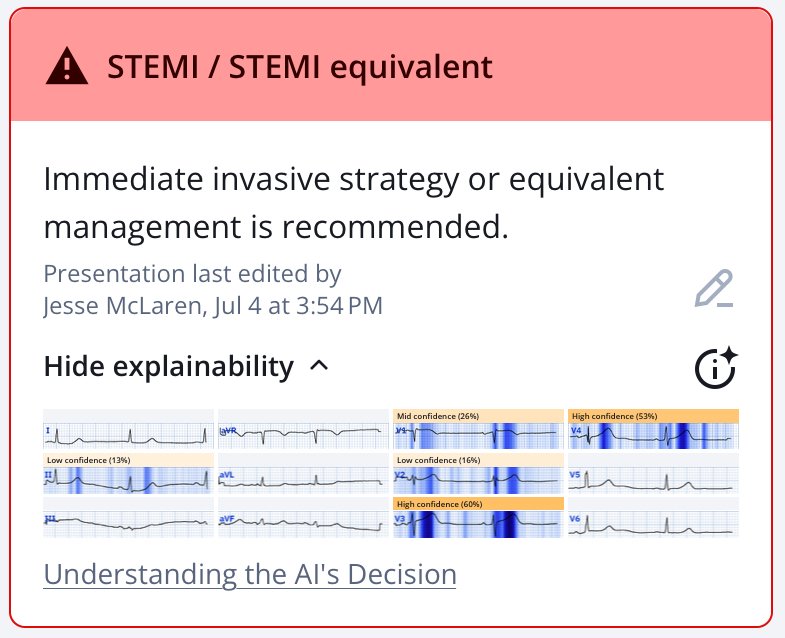
6. Pain is improved (even if still present)!! Even without any of the prior ECGs, documenting an improvement in ischemic chest pain from 7/10 to 3/10 is the same as confirming that the patient has ongoing, refractory chest pain (along with a rising troponin) – which is an indication for immediate reperfusion according to Non-STEMI guidelines – but which is rarely followed.
Instead, the patient was treated as most Non-STEMI: “trend” troponins and plan for non-urgent angiogram. Troponins increased to 300 then 1500, and the patient was given a nitro patch. The trop continued to increase to 1700 then 2500 ng/L, and the nursing notes indicate the patient continued to have mild ongoing chest pain.
There were no further ECGs until 12 hours after arrival, when the patient arrested:
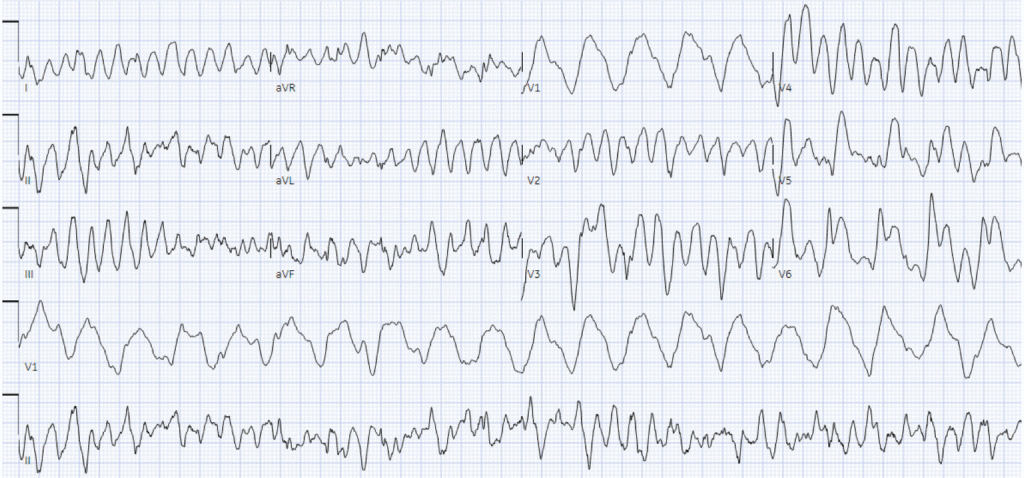
Polymorphic VT, treated with CPR and defibrillation:
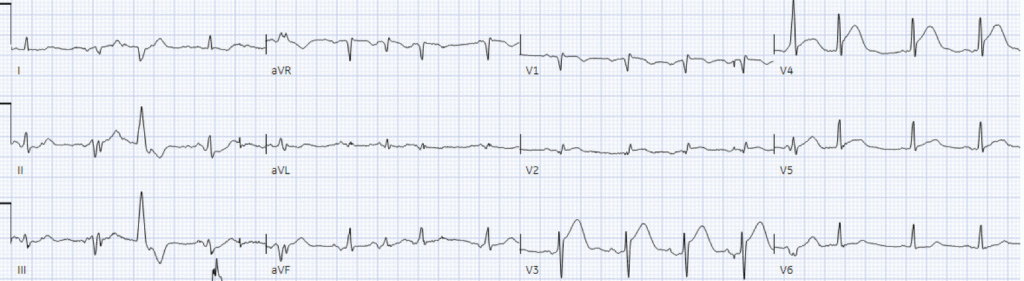
Ongoing hyperacute T waves and new ST elevation in V3-4.
Cardiac arrest was lucky! If the patient hadn’t arrested, they would have continued to quietly lose myocardium, and reperfusion would have been further delayed. Although by 12 hours, almost all the benefit of reperfusion is lost. But because their post-arrest ECG finally met STEMI criteria, the cath lab was activated and there was a 100% proximal LAD occlusion.
Using the Queen of Hearts, this patient could have had immediate cath lab activation at triage, even before their first troponin came back normal. Instead, door-to-cath time was 13 hours, peak troponin was 24,000 ng/L, and EF was 40% with severe hypokinesis of the anterior wall. Post-cath ECG showed anterior reperfusion T wave inversion:
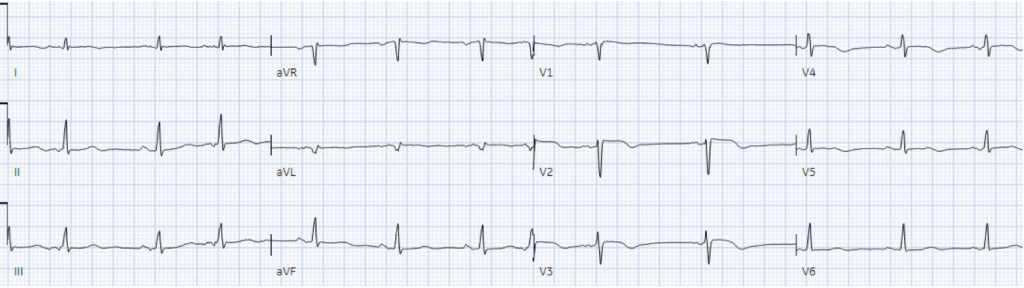
In summary, to answer the question “to cath or not to cath”:
- No STEMI criteria on serial ECGs: But STE has poor sensitivity for OMI, and there were hyperacute T waves
- No reciprocal change: Not all LAD occlusions have inferior STD, and there was precordial swirl
- First troponin was normal: Troponin is a rear-view mirror, which only shows damage in the past, so it is often normal in OMI
- Second trop not high enough: troponin gets “trapped” behind an occluded artery and often remains low until released by reperfusion.
- No evolution of to ST Elevation? This is common in all OMI, including LAD OMI. Hyperacute T waves often do not progress to STE. And, besides that, there were dynamic changes.
- Pain improved with nitro: That is not good enough. It did not resolve. Any MI (OMI or NOMI) with persistent ECG ischemia and/or persistent pain is an indication for emergent cath lab. (The only acute OMI that is not would be one that is reperfused, but even tht is risky). Besides, continued infarction also leads to diminished pain, as there is less viable myocardium that is painful!!

=====================
======================================
MY Comment, by KEN GRAUER, MD (7/7/2025):
Today’s telling post by Dr. McLaren consolidates many of the KEY reasons that all-too-many clinicians continue to miss the opportunity for optimal intervention in patients who present with new CP (Chest Pain). The unfortunate result is too much lost myocardium.
- Improvement is needed …
For clarity in Figure-1 — I’ve reproduced the initial ECG in today’s case, which I’ve put together with the 2nd repeat ECG that was done 2 hours later.
- Question: Which lead(s) in today’s initial ECG do we know can not possibly be normal in a patient with new CP?
====================
Figure-1: I’ve put today’s initial ECG together with the 2nd repeat ECG that was done ~2 hours after the initial tracing.
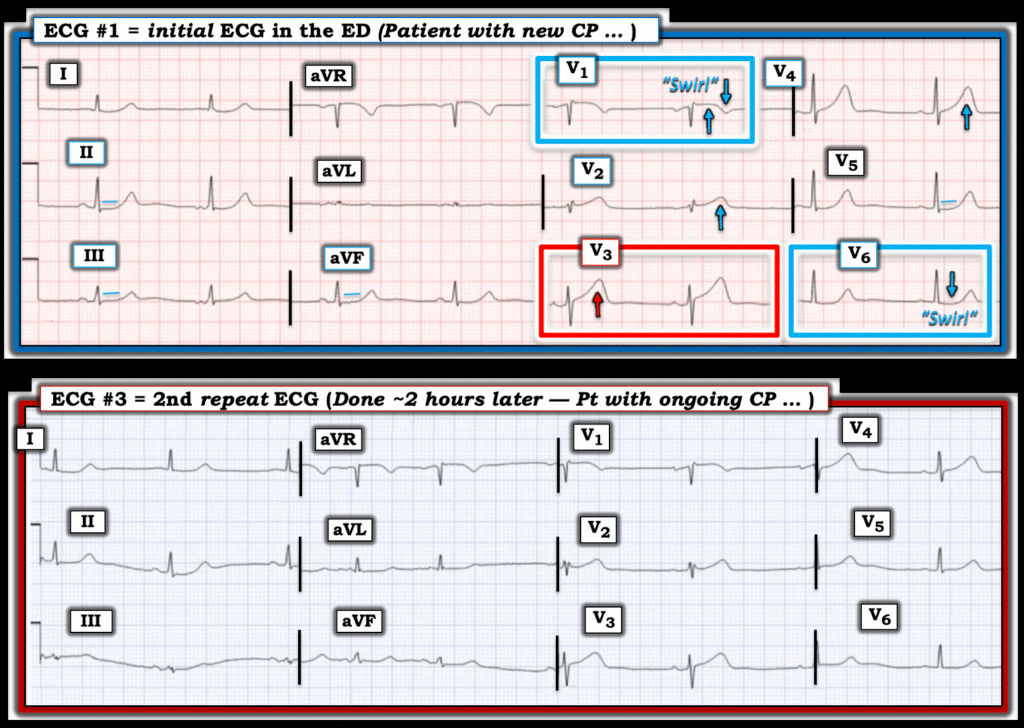
================================
ECG #1: Which Leads Can Not Possibly be Normal?
Regardless of whether you use the QOH (Queen Of Hearts) application to assist in your recognition of acute ECG changes, or simply learn to recognize the patterns — there is simply no way in a patient with new CP that the ST-T wave in lead V3 of the initial ECG can be normal.
- Not only is the T wave in lead V3 taller than the R wave in this lead — but this T wave is decidedly “bulkier” than-it-should-be (“fatter”-at-its-peak and wider-at-its-base than what one would expect given modest size of the QRS in this lead).
- By the concept of neighboring leads — the T waves in neighboring leads V2 and V4 are also clearly “bulkier” than they should be. Keeping in mind that today’s patient presented with persistent severe new CP — our “threshold” for calling ST-T waves “abnormal” has to be substantially lowered in this patient at higher risk for an acute cardiac event. As a result — the ST-T waves in these 3 mid-chest leads have to be labeled hyperacute until proven otherwise!
- But there is more! In fact — almost all leads in this initial ECG are abnormal. Given the higher risk history — and the finding of hyperacute ST-T waves in leads V2,V3,V4 — our “threshold” for calling more subtle ST-T wave findings abnormal has to be lowered.
- As per Dr. McLaren — the ST-T wave appearance in leads V1 and V6 is consistent with Precordial “Swirl” (subtle but definitely abnormal ST elevation for lead V1, with surprisingly deep T wave inversion in this lead — and ST segment flattening with subtle-but-real ST depression in lead V6).
- Confirming this “Precordial Swirl” pattern in ECG #1 — Isn’t the slightly coved ST elevation with deep terminal T wave inversion in lead V1 — the precise mirror-image opposite ST-T wave picture as we see for the slightly bent and depressed ST segment with terminal T wave positivity in lead V6? (Check out the October 15, 2022 post for numerous examples of “Swirl” patterns — with summary in My Comment at the bottom of the page for Pearls on ECG recognition).
- This leaves us with lead V5 in the chest leads. We know the ST-T wave in this lead is also abnormal — because of how flat the ST segment is. But isn’t this exactly as we might expect for a “transition” lead, given the slightly elevated ST segment in neighboring lead V4 — and the ST depression that follows in lead V6?
- ST-T wave changes are more subtle in the limb leads — but having “honed” our eyes in seeking out ST-T wave abnormalities in each of the 6 chest leads — it should be easy to appreciate abnormal ST segment flattening in leads I,II,III; aVL and aVF (with slight ST depression in leads I and II).
- To Emphasize: In the absence of hyperacute findings in the chest leads — these more subtle ST-T wave abnormalities in the limb leads of ECG #1 would probably be interpreted as nothing more than “nonspecific” changes. But in the context of the above noted chest lead abnormalities — these limb lead findings are supportive of the overall picture.
BOTTOM Line: As per Dr. McLaren, regardless of the rationale provided for the “5 Common Reasons Not to Cath” — in this patient who presents with severe new CP — today’s initial ECG is diagnostic of acute proximal LAD occlusion until proven otherwise. Prompt cath with PCI is clearly indicated — even without need for additional evaluation.
================================
PEARL: As per Dr. McLaren — “dynamic” ST-T wave changes were not detected by providers on follow-up ECGs. But — Isn’t it EASY to pick up significant differences in ST-T wave size and “volume” between ECG #1 and ECG #3 when you compare ST-T wave appearance by looking lead-to-lead?
- Even accounting for a slight leftward frontal plane axis shift (ie, the QRS was all positive in lead III of ECG #1 — whereas there is a null vector in lead III of ECG #3) — ST-T waves in ECG #3 have decompressed (shrunk in size) compared to ECG #1 in leads II, aVF; and V3,V4,V5,V6 — with resolution of S depression in lead V6.
- In my experience, the reason providers most often fail to appreciate subtle-but-real “dynamic” ST-T wave changes — is that they do not go lead-by-lead with both tracings placed next to each other when they compare serial tracings.
===================================
Final IRONY in Today’s Case: Total door-to-cath time in today’s case was 13 hours — despite the fact that from just the history and the initial ECG, the indication for prompt cath was immediately established (even before the 1st Troponin value returned from the lab).
- It wasn’t until 12 hours later when the patient had cardiac arrest and manifested ST elevation on the post-resuscitation ECG — that the decision was finally made to perform cardiac catheterization. Were it not for this cardiac arrest — cardiac cath would probably not have been performed for many more hours.
- But despite deleterious effects from this delay in reperfusion — chart documentation will show that cardiac catheterization was performed within less than an hour “after STEMI criteria were satisfied”. The irony will be that on the chart — it will look like this patient received “great care” by performance of cardiac cath within an hour of satisfying STEMI criteria (which will erroneously reinforce “validity” of the outdated and flawed STEMI paradigm — when in fact, it was adherence to STEMI criteria in the first place that resulted in this patient’s cardiac arrest).