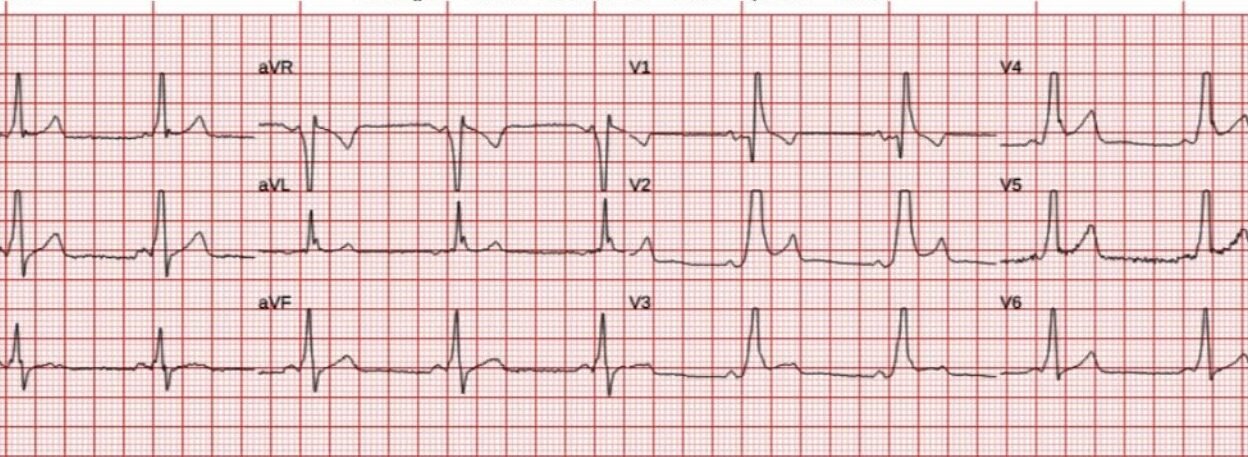
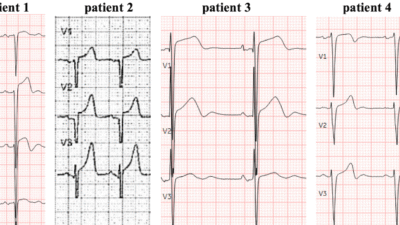
A man in his 50s had chest pain and shortness of breath. EMS arrived and recorded this ECG.
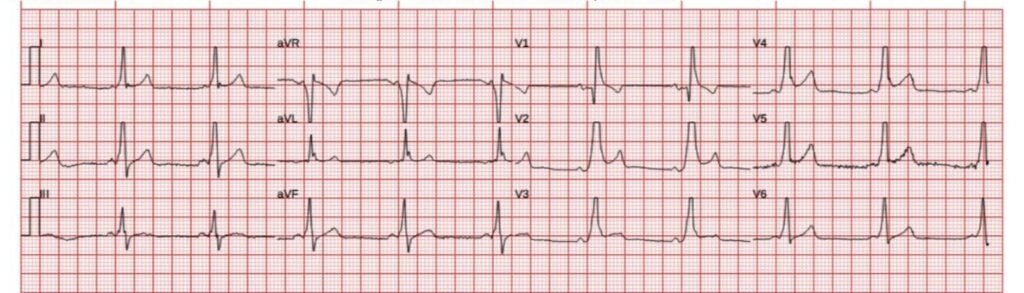
What do you think?
There is sinus rhythm with preexcitation causing abnormal QRS complexes, and consequently, abnormal repolarization. There is concordant STE in V2-V5, however this is something I have observed occasionally in WPW. The T waves are not hyperacute. I would favor WPW causing a STEMI mimic pattern, but it could be baseline WPW with superimposed anterior acute transmural injury.
Zoll interpretation on EMS monitor included “***STEMI***”
Queen of hearts interpretation:
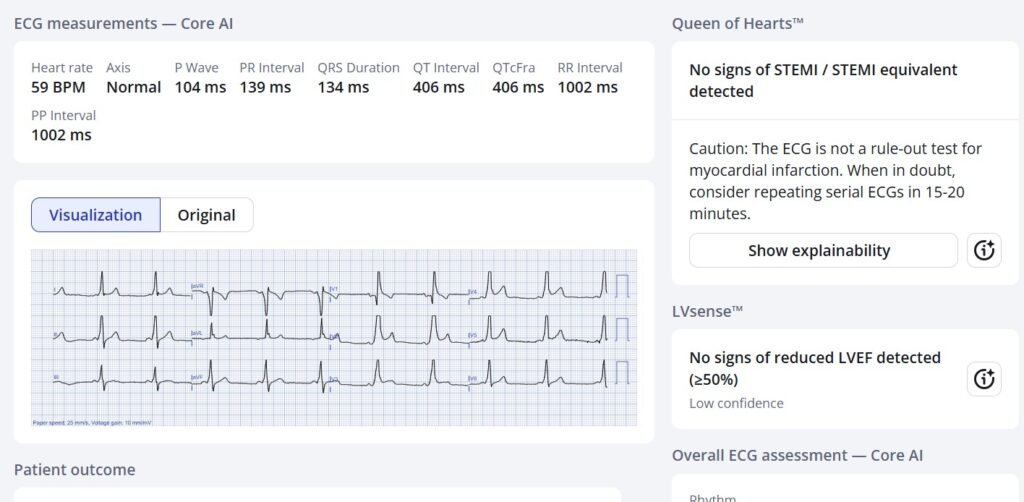
PMcardio for Individuals now includes the latest Queen of Hearts model, AI explainability (blue heatmaps), and %LV Ejection Fraction. Download now for iOS or Android: https://individuals.pmcardio.com/app/promo?code=DRSMITH20. As a member of our community, you can use the code DRSMITH20 to get an exclusive 20% off your first year of the annual subscription. Disclaimer: Certain AI ECG Modules are CE-marked medical devices under EU MDR and are certified for marketing only in the European Union and the United Kingdom. PMcardio technology has not yet been cleared by the US Food and Drug Administration (FDA) for clinical use in the USA.
The cath lab activation was cancelled after discovering the patient had a known history of WPW and a prior ECG was available:
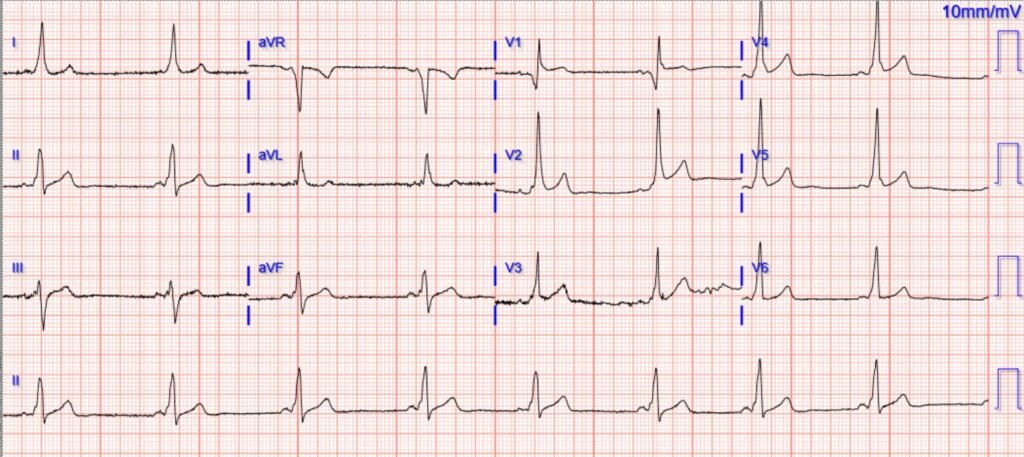
Troponins were negative.
No other dangerous cause of symptoms was discovered and the patient did well.
Other WPW related posts:
It is easy to be led astray by the computer….
It is easy to be led astray by the computer….
https://drsmithsecgblog.com/repost-certain-pattern-of-pseudostemi/
= = =
======================================
MY Comment, by KEN GRAUER, MD (11/28/2025):
The incidence of WPW (Wolff-Parkinson White) Syndrome is ~2/1,000 in the general population (Chhabra et al — StatPearls, 2023). This means that although this syndrome is not overly common — it occurs often enough to ensure that every health care provider who deals with ECGs will at least occasionally encounter this syndrome. There are 2 principal reasons why familiarity with this syndrome is especially important for emergency providers:
- Reason #1: WPW is often associated with cardiac arrhythmias — due in large part to availability of an AP (Accessory Pathway) that facilitates reentry tachycardias and exceedingly rapid conduction with atrial fibrillation or atrial flutter. Fortunately, the vast majority of patients with WPW have an excellent long-term prognosis — and, the overall incidence of sudden death with this syndrome is extremely low. That said, WPW-related arrhythmias can be potentially life-threatening — because extremely rapid rates (over 250/minute) may be attained if a patient with WPW develops AFib or AFlutter. These excessively rapid rates can precipitate deterioration of the rhythm to VFib.
- Reason #2: WPW is often thought of as the “Great Mimic” of other conditions. The presence of QRS widening with resultant secondary repolarization changes in the ST-T wave may produce an ECG picture that simulates RBBB, LBBB, IVCD, LVH, RVH, and/or myocardial infarction or ischemia.
= = =
Today’s Initial ECG:
Today’s case by Dr. Meyers addresses Reason #2:
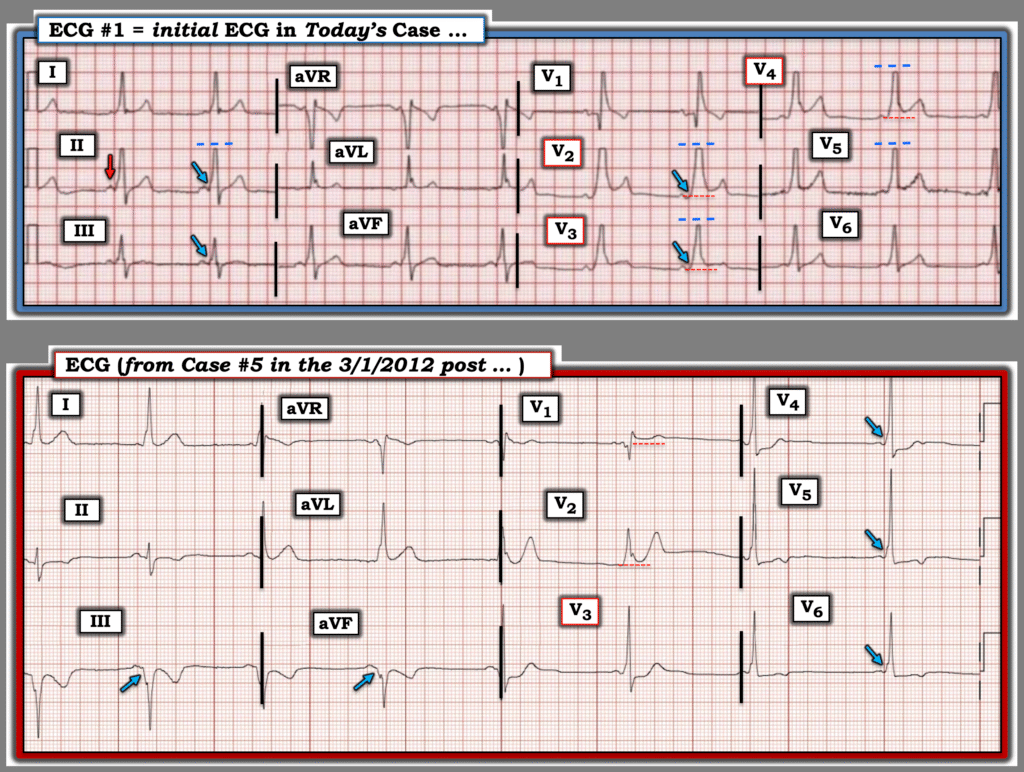
- For clarity in Figure-1 — I’ve reproduced and labeled today’s initial ECG, and compare this tracing to another example of WPW previously published in Dr. Smith’s ECG Blog.
- As per Dr. Meyers — today’s initial ECG shows the 3 components of WPW: i) Sinus rhythm with a short PR interval (RED arrow upright P wave in lead II) — ii) Delta waves (BLUE arrows showing some of the delta waves on the 2 tracings in Figure-1) — and, iii) QRS widening.
- The concern with today’s initial ECG (Top tracing in Figure-1) — is the abnormal ST elevation in multiple chest leads (RED dotted lines in leads V2,3,4). Even though R wave amplitude is clearly cut off in leads V2-thru-V5 of this pre-hospital tracing (dotted BLUE lines in these leads, as well as in lead II) — this concordant ST elevation in the above chest leads would not normally be expected given the entirely positive QRS complexes in these leads.
- BOTTOM Line: Dr. Meyers appropriately concluded that although WPW with a “STEMI-mimic pattern” seemed the most probable explanation — that it was impossible on the basis of this single ECG to rule out anterior infarction superimposed on a WPW baseline tracing. Fortunately, a prior ECG was found on today’s patient that confirmed that there were no acute changes compared to this patient’s baseline ECG.
= = =
What about the Bottom ECG in Figure-1?
By way of comparison — I added another example of WPW from Dr. Smith’s ECG Blog (this being the 2nd ECG from Case #5 in the March 1, 2012 post — in which this patient was awakened from sleep by new-onset chest pain).
- Once again — there is sinus rhythm with a shortened PR interval (best seen in the chest leads) — QRS widening — and multiple delta waves (some of which I’ve highlighted with BLUE arrows in this 2012 tracing).
- Once again — there is a completely positive QRS complex in lead V2 with concordant ST elevation in this lead (RED dotted line in V2).
- What else do YOU see in Figure-1 from this 2012 ECG?
= = =
Figure-1: Comparison between the initial ECG in today’s case — with an ECG from Case #5 in the March 1, 2012 post in Dr. Smith’s ECG Blog.
= = =
ANSWER (What else in this 2012 ECG?)
My “eye” was drawn to the following additional findings:
- In addition to the ST elevation in lead V2 — the upright T wave in this lead is huge with respect to the QRS in V2.
- There is also ST elevation in lead V1.
- The shape of the depressed ST segment in lead V3 (and to a lesser extent, also in lead V4) — is flat and “shelf-like” (similar in shape and location to the ST depression we see with posterior OMI).
- The concordant T wave inversion in lead III looks “bulkier” than what I would normally expect.
“My Take” — It’s hard to make “rules” regarding what the ST-T waves “should look like” in a patient with WPW — because almost anything might be possible as a result of altered depolarization that occurs with activation of the ventricles via travel over an accessory pathway.
- The above said — I look for ST-T wave changes that shouldn’t be there. By this I mean that even with WPW — I would not expect there to be such “shelf-like” ST depression as we seen in lead V3 (and by extension — in lead V4). Similarly — the concordant ST elevation in lead V2 would not normally be expected, especially in association with such a disproportionately enlarged T wave in this lead.
- This said — it will often not be easy to assess the ECG of a patient with WPW who presents with new chest pain. In such cases — verification of our suspicion by: i) Looking for a prior ECG on the patient; — ii) Doing a couple of serial ECGs to see if there are “dynamic” changes; — iii) Checking at least 2 Troponins; — and, iv) Doing a bedside Echo (ideally while the patient is still having chest pain — looking for a localized wall motion abnormality) — are prudent actions that will hopefully confirm the diagnosis.
- Follow-Up.: The patient in this Case #5 from 2012 was found to have acute occlusion of the 1st Diagonal branch of the LAD on cardiac catheterization.
= = =
Final Pointers:
- Take another LOOK at Figure-1. Note in today’s initial ECG — that lead V1 lacks a short PR interval and lacks a delta wave, with a QRS that for all the world looks like RBBB.
- Note in the 2012 tracing — that lead II also lacks a delta wave and has a normal PR interval. It would be easy to miss the WPW if one only used lead II for assessment of the rhythm.
- Delta waves are not always seen in all 12 leads of a patient with WPW. While delta waves are seen in almost all leads for the 2 tracings in Figure-1 — they are lacking in lead V1 (Top ECG) and in lead II (Bottom ECG) despite leads II and V1 normally being the best leads for assessing atrial activity, and therefore the PR interval.
= = =
= = =