This was provided by Mustafa Alwan, an internist from Jordan, on Facebook EKG Club
A 50-something female presented with atypical chest pain described as stabbing, with no radiation
PMHx : DM poorly controlled
VITAL signs stable
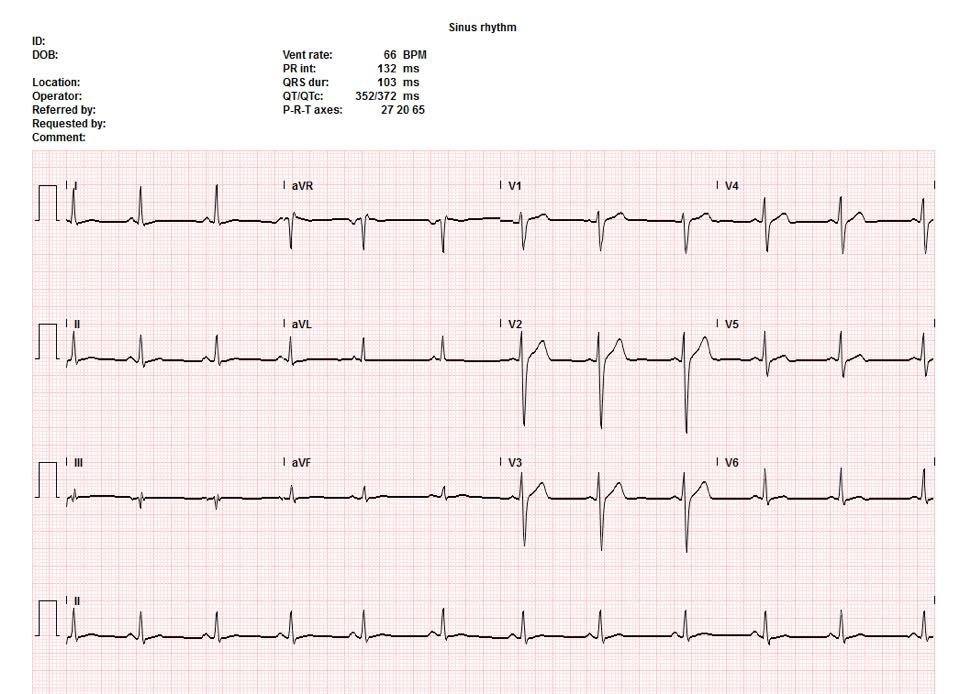
Here is the initial ECG with the question “should the cath lab be activated?”
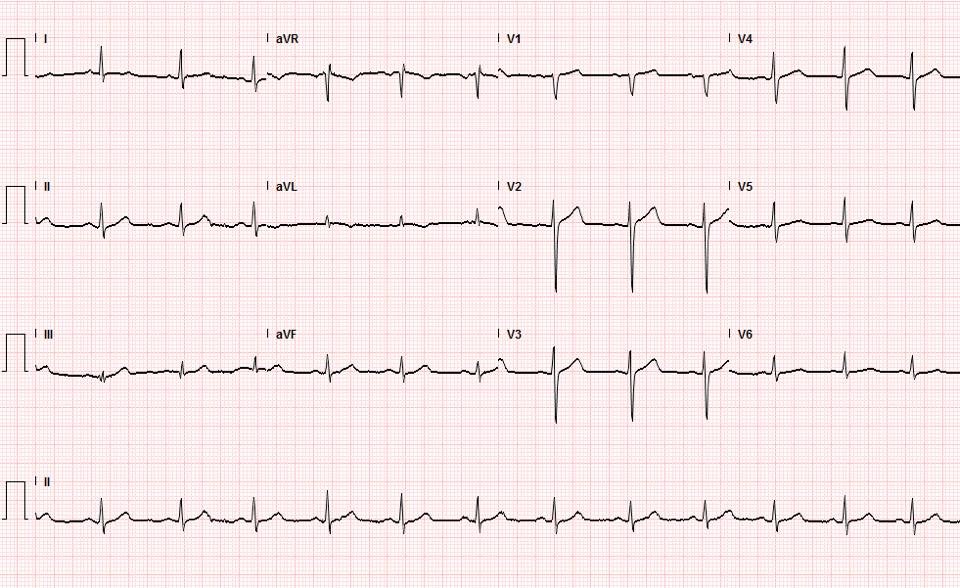 |
| This is suspicious for ischemia because of the T-wave inversion in aVL. However, this is very nonspecific and one would not activate the cath lab! |
Another ECG was recorded 20 minutes later:
See these cases for the importance of ST segment monitoring:
https://drsmithsecgblog.com/search/label/ST%20Segment%20Monitoring
A third ECG was recorded at 45 minutes:
 |
| Now it is unequivocally diagnostic of inferior MI, even though it does not meet millimeter criteria for inferior STEMI. The cath lab must be activated. |
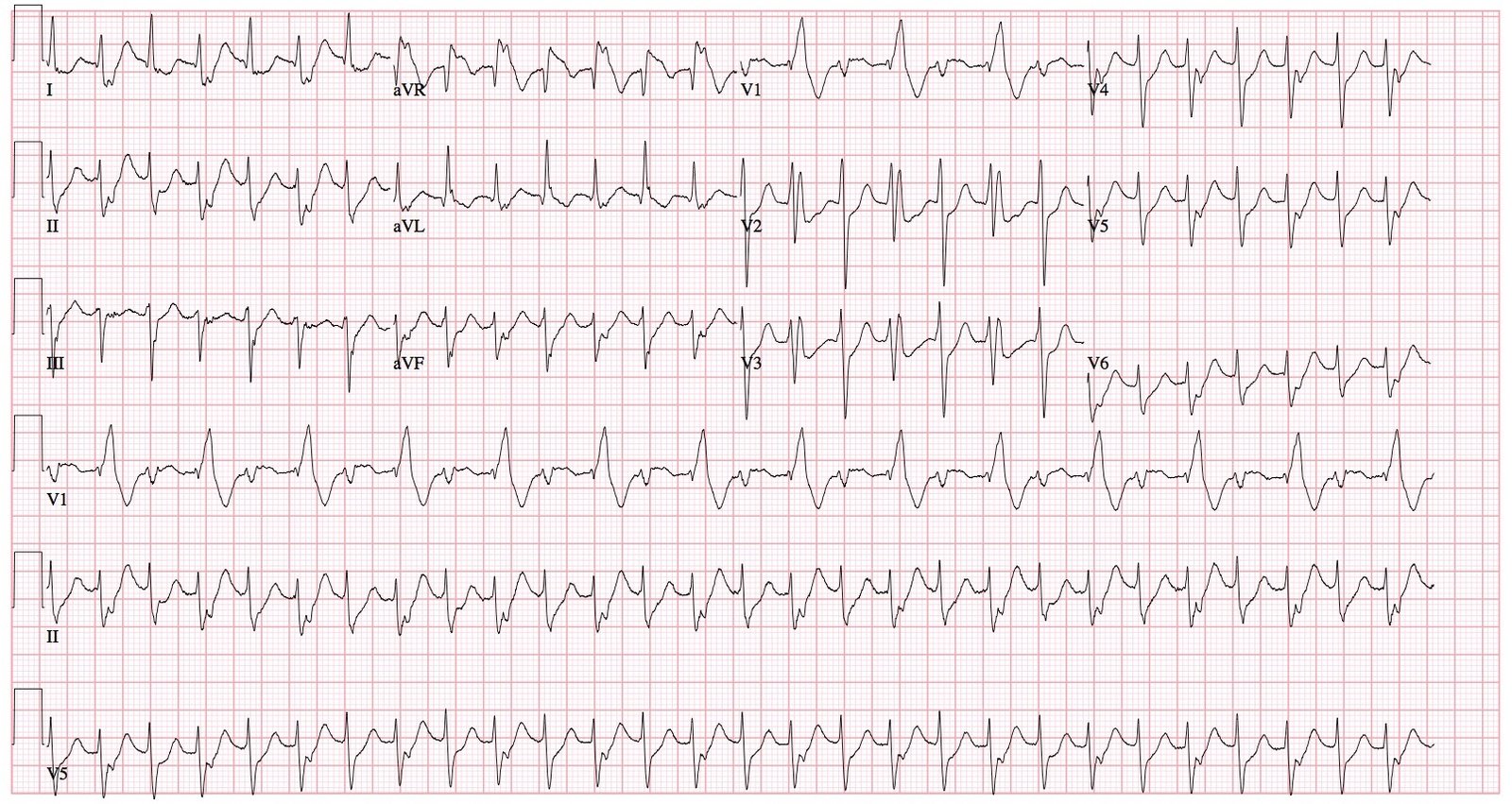
Here are all 3 ECGs, one after another, so you can see the changes:
The cath lab was not activated, but a 4th ECG was recorded at one hour:
 |
| Now it meets STEMI criteria. Cath lab was activated What else do you notice? |
There is also new ST elevation in V1. So this is a right ventricular MI also
Echo: Basal inferior wall hypokinetic, pseudonormal LV filling pattern
Initial Troponin T: less than 0.01 ng/mL initial
Troponin T after 2 hours: 0.49 ng/mL
Troponin T after 4 hours: 1.6 ng/mL (this is a large MI)
Cath showed a 100% proximal RCA occlusion.
Learning Points:
1. T-wave inversion in aVL may be the first sign of inferior MI
2. Pay attention to slightly enlarged T-waves
3. When you see these subtle, nonspecific abnormalities, make certain you get serial ECGs!
4. Any patient with ongoing potentially ischemic chest pain should get serial ECGs!