This was sent by a paramedic who wishes to remain anonymous.
911 was called because a 12 year-old female had a “seizure” at the gym.
On arrival, medics found the patient supine on gym mats, conscious but lethargic. Her skin was very pale, cold, and diaphoretic, and there was no radial pulse but only a palpable brachial. Her lips were cyanotic and firefighters had already begun oxygen therapy. She complained of nausea and bilateral rib pain not worsened by palpation or inspiration. She did not have any obvious injuries on exam, but we noticed bladder incontinence. She was still cyanotic 15 minutes after the “seizure.”
The patient’s coaches stated that she was “warming up” for practice when she suddenly lost consciousness, fell, and had brief seizure-like activity. They denied seeing her sustain any other injuries aside from a ground-level fall onto a soft surface. She regained consciousness within a few minutes, but remained altered.
Later on during transport, the patient was able to recall what happened: she was running when she became very dizzy and lost consciousness. The patient’s family stated that she had no medical history, no previous seizures or similar episodes with exercise, and no family history of cardiac problems or sudden death.
A monitor strip showed frequent PACs.
After a quick exam and history we took her out to the ambulance, where her first set of vitals were: BP 100/63, HR 72, SpO2 99%, RR 22. Her lungs were clear and she never complained of dyspnea.
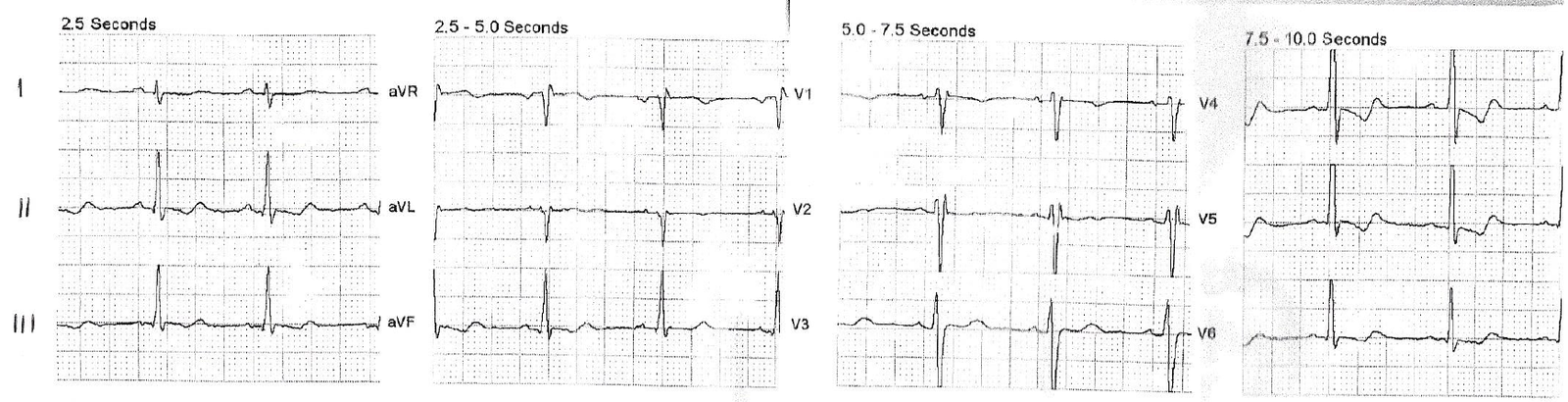
A prehospital 12-lead was recorded:
Case Continued:
After about 6 or 7 minutes on oxygen, the patient’s cyanosis resolved and so did the premature beats. Her mental status and skin greatly improved. However, for the remainder of transport her systolic blood pressure remained in the 80s (86/56) despite improvement otherwise (I wondered later if the first BP was an incorrect reading). We started a fluid bolus and by the time we reached the ED, her only complaint was fatigue.
She was admitted to a children’s hospital.
The followup was somewhat sketchy, as it did not come from medical records but from family via a third party:
She was found to have an anomolous left main coronary artery which reportedly became “pinched” during exercise, causing severe ischemia with drop in cardiac output and syncope.
She had surgery to move the artery and is reportedly doing well. They are just having difficulty keeping her inactive.
Learning Points:
1. It may help to record an ECG in cases of “seizure”
2. Syncope in children can be due to ischemia, as well as due to pure rhythm disturbances such as long QT, WPW, Catecholaminergic polymorphic VT (CPVT), Brugada, AV block, etc.
3. Syncope during activity is particularly worrisome.
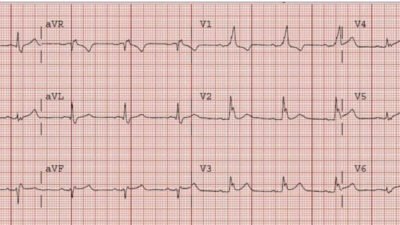
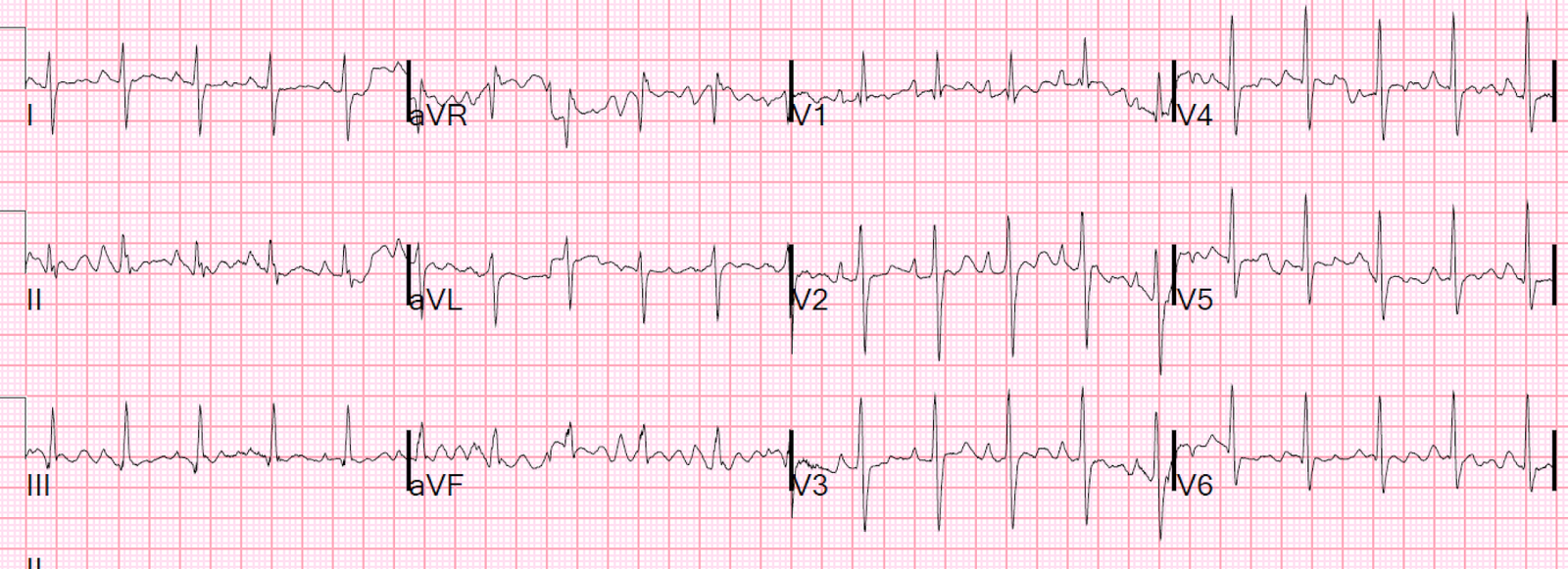
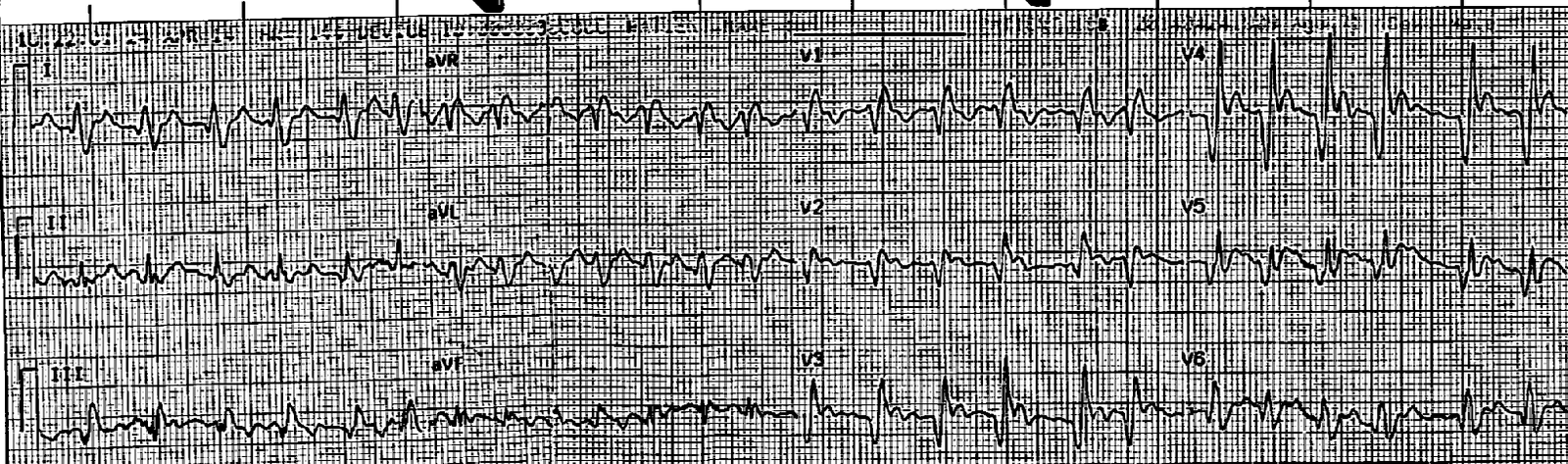
Check out this case:
A 16 year old girl has syncope while playing basketball…..
Here is my article on ED Syncope Workup: