Written by Pendell Meyers, sent by anonymous
A man in his 40s called EMS for acute symptoms including chest pain, abdominal pain, nausea, and diarrhea.
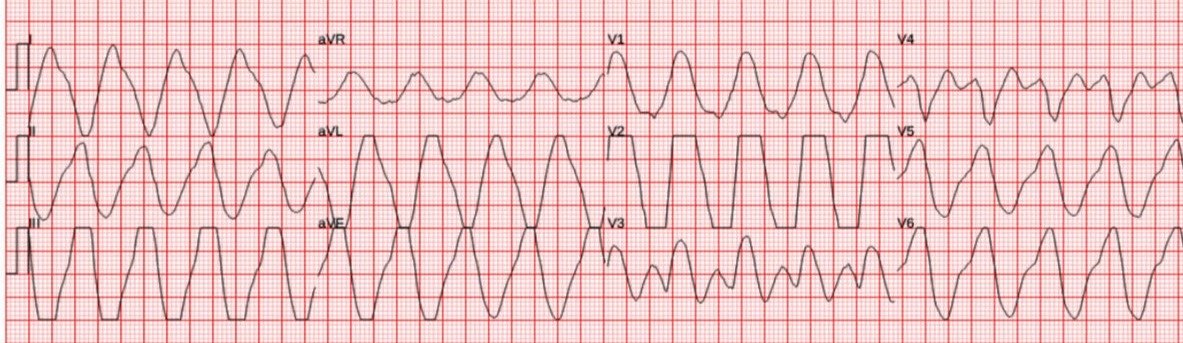
Here is his EMS ECG:
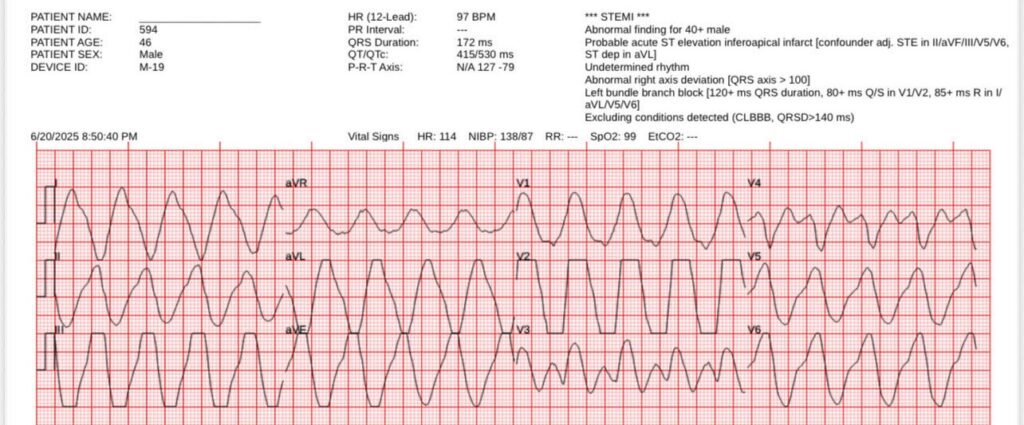
Critical hyperkalemia, with sine wave appearance. Please try to ignore the Zoll machine’s “***STEMI***”!
PM Cardio Queen of Hearts does not cause a false positive STEMI alert in this case:
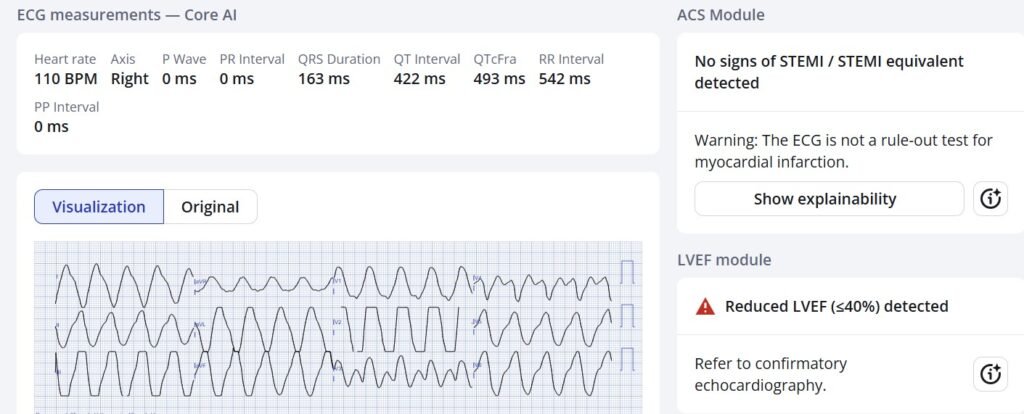
New PMcardio for Individuals App 3.0 now includes the latest Queen of Hearts model and AI explainability (blue heatmaps)! Download now for iOS or Android. https://www.powerfulmedical.com/pmcardio-individuals/ (Drs. Smith and Meyers trained the AI Model and are shareholders in Powerful Medical.)
Paramedics administered 2gm calcium gluconate and continuous albuterol nebulizer, followed by this repeat ECG:
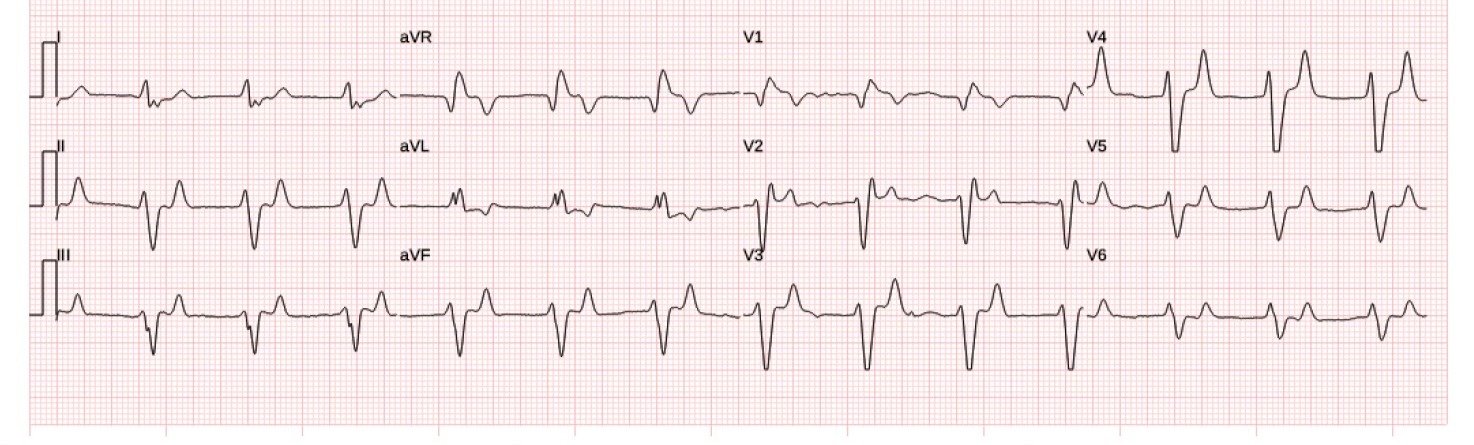
Much improvement in width and morphology, but still more improvement could likely be achieved with more calcium.
On arrival to the ED, the bedside venous blood gas revealed a potassium level of 9.1 mEq/L.
An old ECG from weeks ago was available for comparison:
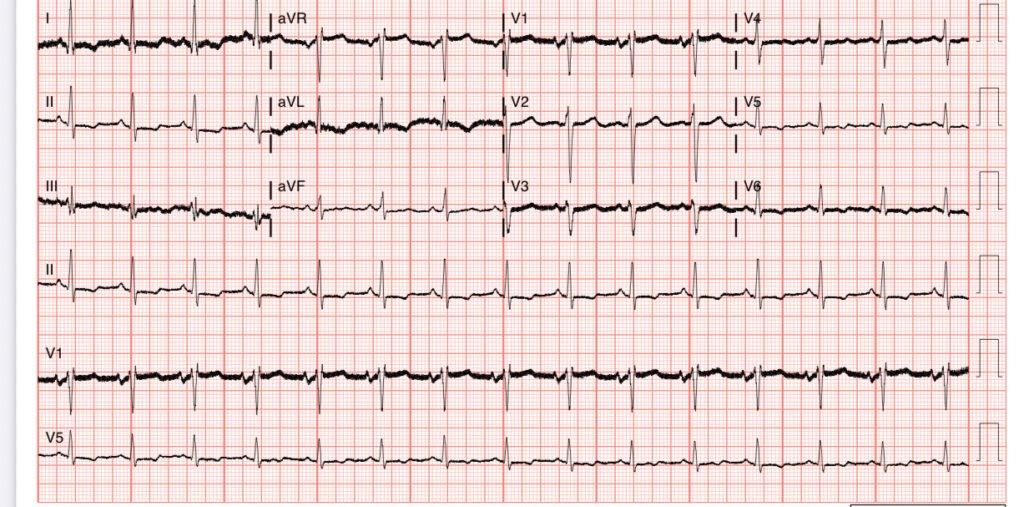
The patient had missed dialysis, complicated by a dysfunctional AV graft.
More calcium was administered, as well as insulin and glucose.
Here is a repeat ECG:
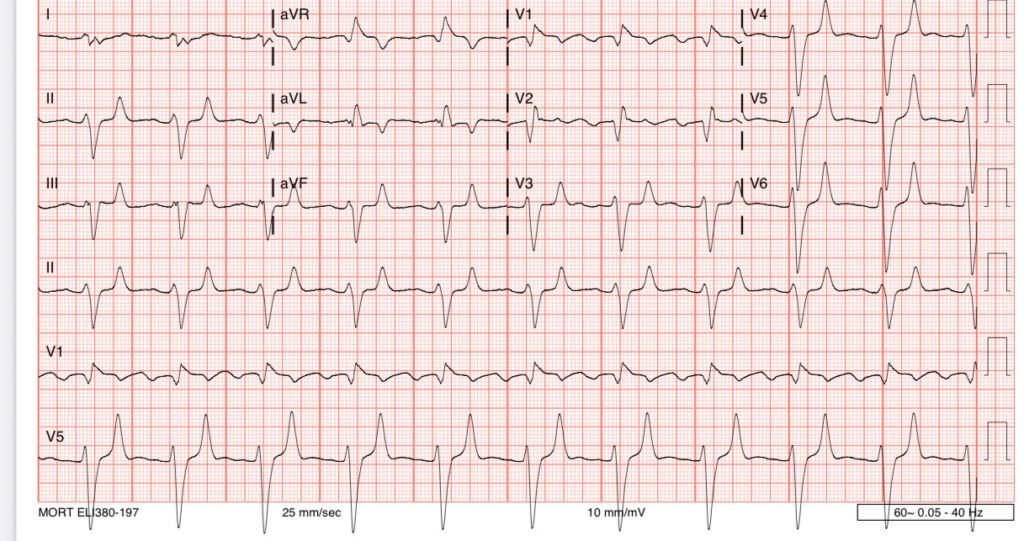
An emergent dialysis access catheter was placed, and dialysis was successful. The patient survived.
======================================
MY Comment, by KEN GRAUER, MD (7/14/2025):
A good general rule is that IF a patient presents with stable vital signs and an ECG that looks, “too wide (and/or too unreal) to be true” — that the reason for this appearance is likely to be either: i) Artifact; or, ii) Hyperkalemia.
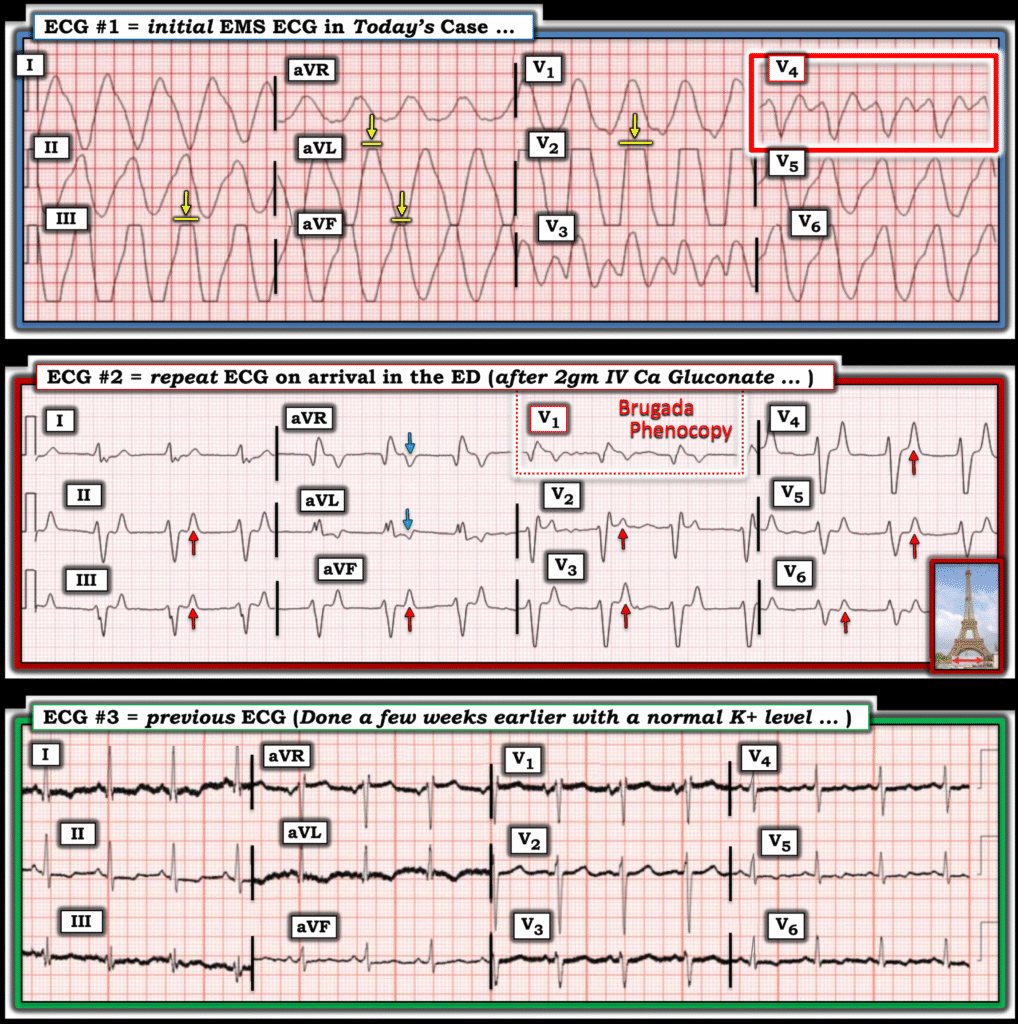
- In today’s case — the paramedics presumably knew the ECG was correctly recorded (and/or perhaps they were able to elicit some history from the patient predisposing to renal insufficiency). This left hyperkalemia as the most likely explanation for today’s initial ECG (that I’ve reproduced in Figure-1).
- Of the 12 leads in ECG #1 — it is lead V4 (within the RED rectangle in ECG #1) that caught my attention as looking “real”, albeit with a dramatically widened QRS complex.
- NOTE: ECG #1 is a prehospital tracing. In the United States (? in other countries) — many of the prehospital ECG machines automatically “cut off” QRS R wave or S wave amplitude that exceeds 10 or more millimeters — which accounts for the straight line appearance in those leads to which I added YELLOW arrows.
- PEARL #1: Be aware that selected patients may manifest surprisingly normal vital signs and alertness despite potentially lethal serum K+ levels (such as the 9.1 mEq/L venous level for the patient in today’s case).
- The EMS Team correctly suspected severe hyperkalemia in ECG #1 as the cause of marked QRS widening without sign of atrial activity (and as a result — they correctly administered empiric calcium gluconate IV).
- To Emphasize (As per Dr. Meyers) — there is no need to verify a low serum level of K+ before giving empiric IV Calcium when the tracing in front of you resembles the initial EMS ECG in today’s case. This ECG is diagnostic of critically elevated serum K+, with need for immediate treatment (and there is no downside to giving empiric IV Calcium in this situation).
For review of the ECG findings of Hyperkalemia — Check out My Comment at the bottom of the page in the January 26, 2020 post in Dr. Smith’s ECG Blog. Many of these findings are seen in ECG #2 (with these findings still present after 2 gm of IV Calcium Gluconate + continuous Albuterol nebulizer). These ECG findings include:
- Marked QRS widening (to ≥0.14 second in ECG #2).
- Absent P waves
- Tall, peaked and pointed T waves in multiple leads (RED arrows in ECG #2 — that highlight an “Eiffel Tower-like” T wave appearance, in which these symmetric, tall pointed T waves manifest a surprisingly narrow base).
- Occasional pointed T waves that are negative (BLUE arrows in ECG #2).
- Brugada Phenocopy (See My Comment at the bottom of the page in the January 13, 2025 post).
Appreciation for the ECG changes of marked hyperkalemia that we see in ECG #1 and ECG #2 — become readily apparent when we compare these tracings to ECG #3, which is a baseline tracing from today’s patient, recorded when serum K+ was normal.