Written by Pendell Meyers
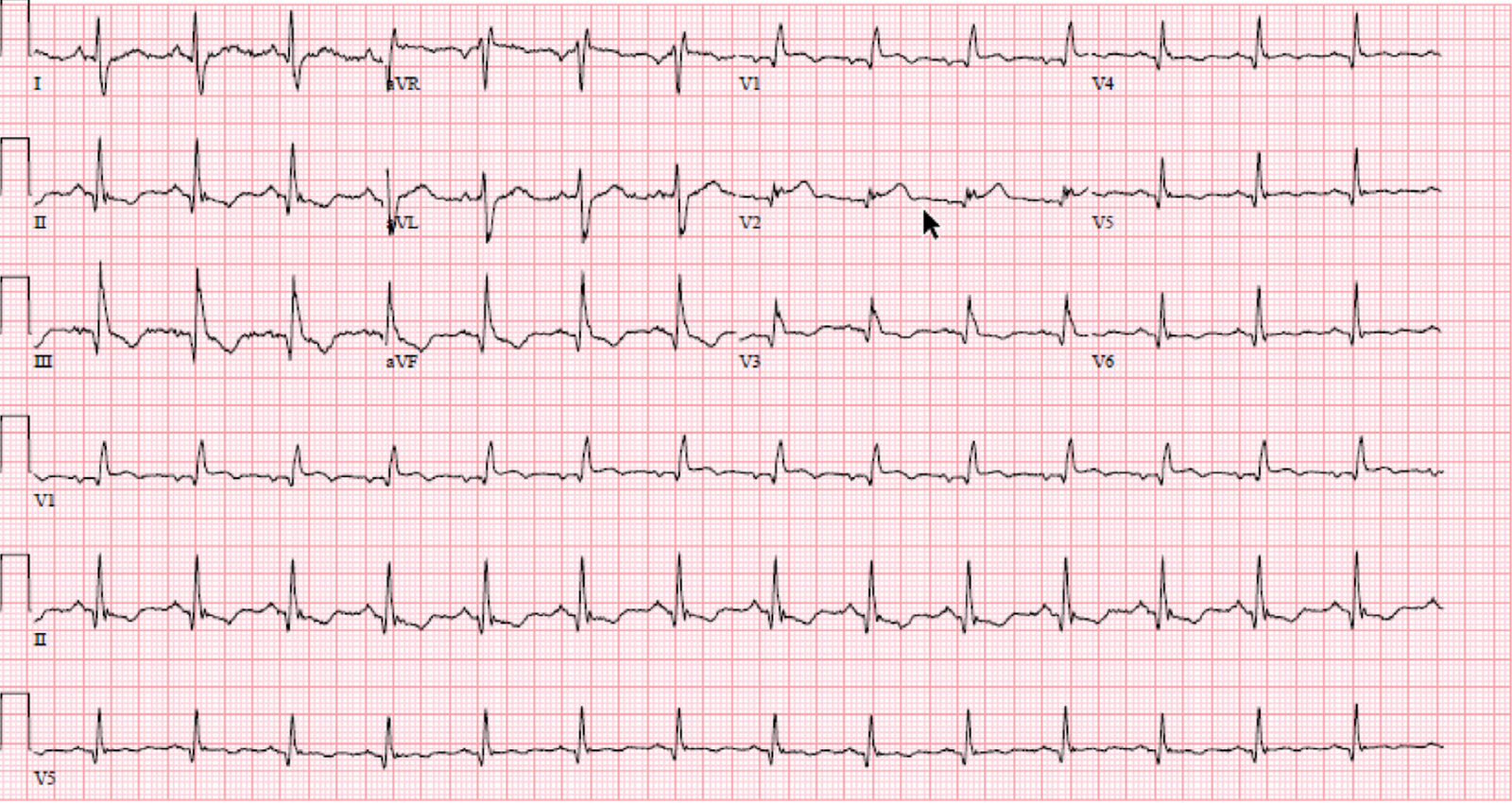
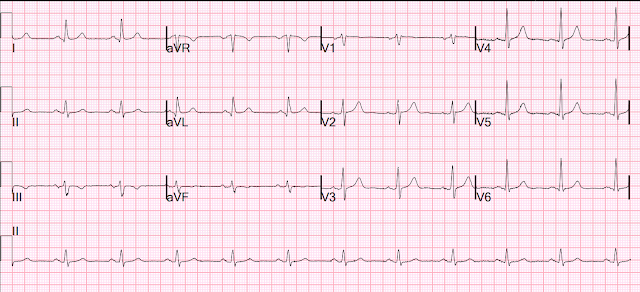
A woman in her 60s had acute chest pain and shortness of breath. EMS arrived and recorded this ECG (no baseline ECG available):
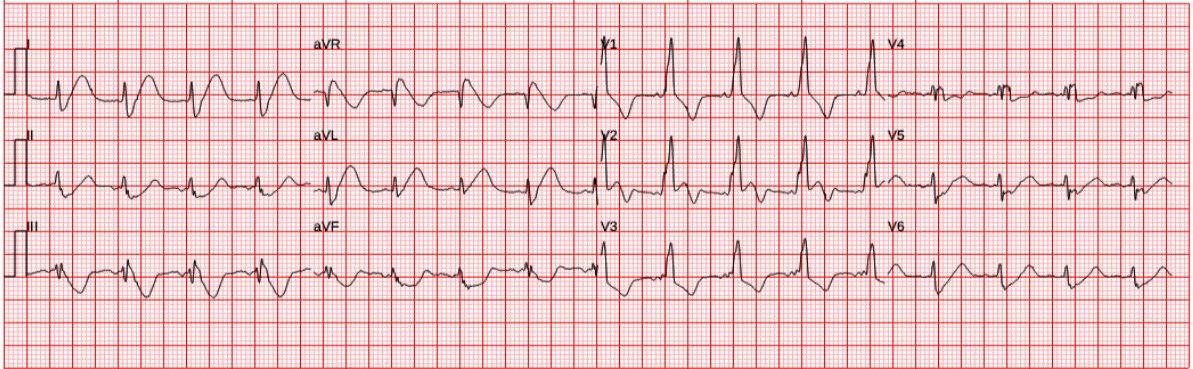 |
| What do you think? |
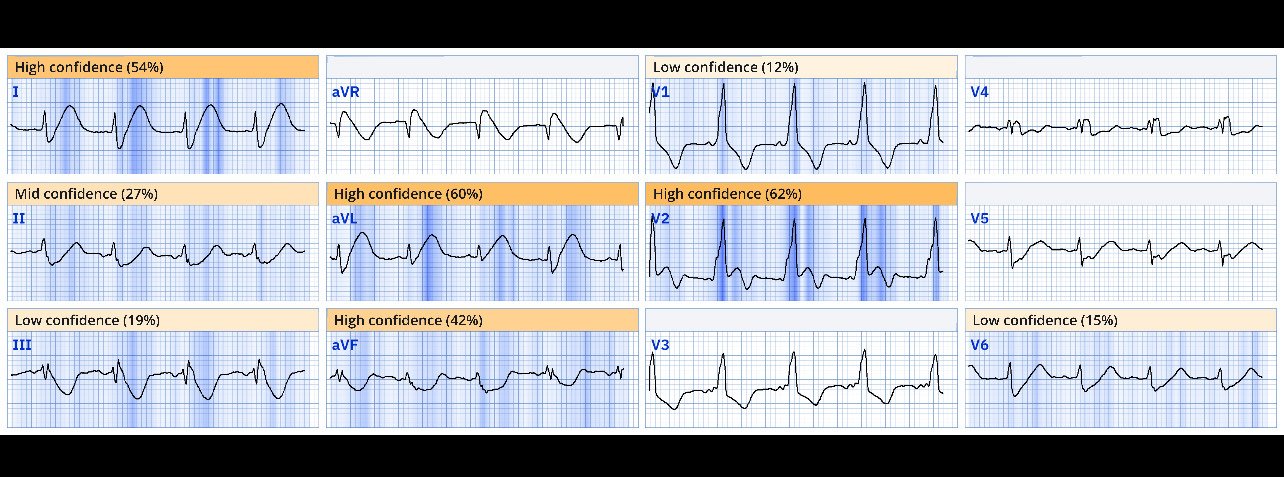
Sinus rhythm, RBBB, and anterolateral OMI pattern with concordant STE in V2, inappropriate STD (precordial swirl pattern) in V5 anv V6, HATW in I and aVL, with reciprocal STD and negative HATW in III and aVF. Proximal LAD OMI would be the most likely cause.
Here is the Queen of Hearts interpretation: STEMI / STEMI equivalent (OMI) with high confidence
This was expertly recognized, and she bypassed the ED and went straight to the cath lab, where a proximal total LAD occlusion was opened.
She did well.
How do we diagnose LAD OMI on the ECG in the presence of Right Bundle Branch Block?
Here is a nice case of chest pain and RBBB, with references, and discussion of RBBB and LAD OMI, written mostly by Smith:
Triska J, George J, Rector G, et al. Acute coronary occlusion in a patient with prior known right bundle branch block: Another chink in the armor for the ST-elevation myocardial infarction criteria. Ann Emerg Med [Internet] 2023;82(2):219–21. Available from: http://dx.doi.org/10.1016/j.annemergmed.2022.12.006 https://emergencymed.org.il/wp-content/uploads/2023/09/Acute-Coronary-Occlusion-in-a-Patient-With-Prior-Known-Right-Bundle-Branch-Block.pdf
===================================
MY Comment, by KEN GRAUER, MD (5/13/2025):
===================================
I reviewed today’s initial ECG knowing only that the patient was a woman in her 60s who contacted EMS for acute CP (Chest Pain) and shortness of breath.
- For clarity in Figure-1 — I’ve reproduced and have labeled this initial ECG.
Interpretation of ECG #1:
As per Dr. Meyers, in this 60s woman with new CP — the ECG in Figure-1 suggests acute LAD OMI until proven otherwise:
- The rate is a bit fast (about 100/minute).
- There is RBBB (Right Bundle Branch Block).
- There are obvious hyperacute ST-T waves in leads I and aVL — as well as an unusual biphasic ST-T wave in lead V2 (double RED arrows in this lead — with the ST elevation in the initial part of the ST segment clearly abnormal given the RBBB that typically results in ST-T wave depression).
- There is equally marked reciprocal ST depression in each of the inferior leads (II,III,aVF) — as well as in lateral chest leads V5,V6.
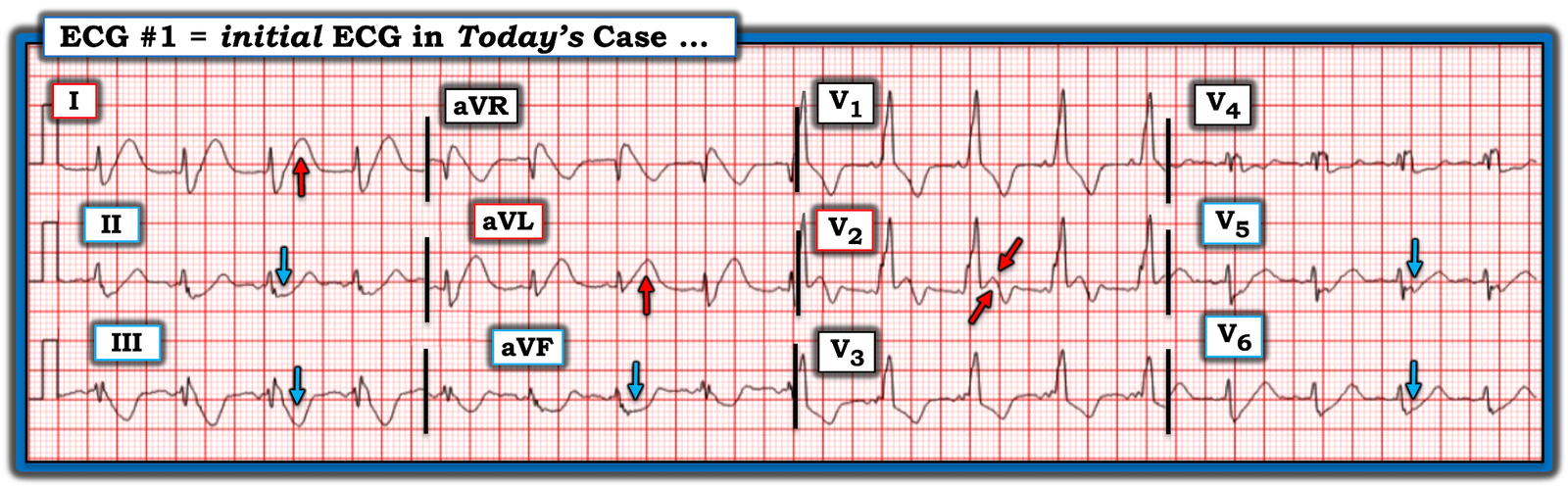 |
| Figure-1: I have labeled the initial ECG in today’s case. |
BUT — Is there WPW?
And then I looked closer at the P wave, PR interval and QRS complex in leads V1,V2,V3 (See BLUE arrows in these leads in Figure-2, in which I have magnified selected leads from ECG #1).
- Doesn’t the PR interval in these anterior chest leads look short? — with in addition, slurring of the initial upward slope of the QRS (simulating a delta wave?).
- KEY Point: Regardless of whether or not today’s patient has WPW — the magnitude of hyperacute ST-T wave changes in multiple leads in this 60s woman with new CP merits prompt cath to define the anatomy.
- WPW is notorious for its potential to manifest pseudo-infarction patterns. And, in those uncommon situations in which a patient with WPW does develop acute MI — alterations in the widened QRS complex and resultant changes in ST-T wave morphology often serve to mask acute ECG findings, making it much more difficult to recognize acute MI on the ECG of a patient with WPW.
- The above said — at times the magnitude of ST-T wave abnormality resulting from an acute MI will be marked enough to suggest an acute event despite the associated presence of WPW (See the July 11, 2014 post — and My Comment at the bottom of the page in the October 13, 2022 post for illustration of these concepts regarding pseudo-infarction vs recognition of acute MI in association with WPW).
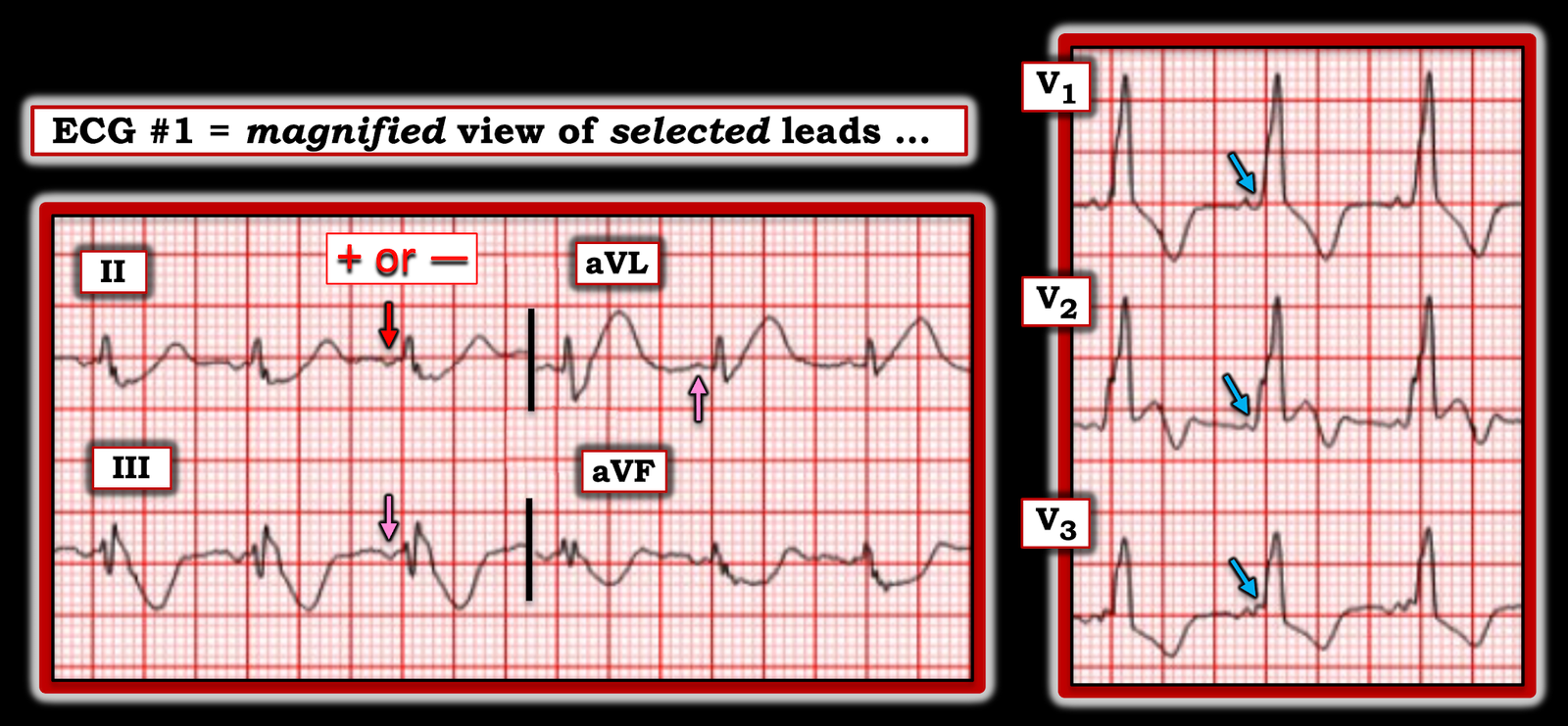 |
| Figure-2: I’ve magnified selected leads from ECG #1. |
WPW is Unlikely . . .
While important to consider the possibility of WPW from the appearance of atrial activity in relation to neighboring QRS complexes in leads V1,V2,V3 — I do not think the ECG in Figure-1 represents WPW.
- While I had no idea about the medical history of today’s patient at the time I reviewed ECG #1 — it’s helpful to keep in mind that discovery of WPW for the 1st time at age 60+ would be rare.
- While the QRS complex in lead V1 of Figure-1 is monophasic (ie, lacking the triphasic rsR’ morphology characteristic of typical RBBB) — there is a slender initial R wave, followed by a wide, terminal S wave in left-sided leads I and V6 — such that QRS morphology in today’s 12-lead tracing is consistent with RBBB.
- The magnified view in Figure-2 — suggests that the P wave in lead II is not upright (RED arrow in this lead). The P wave is also negative in lead III — and positive in lead aVL (PINK arrows in these leads) — which suggests a non-sinus rhythm. As a result — the PR interval might not be short after all, if the site of the atrial impulse arises from a site close to the AV node.
- While the number of leads that manifest definite delta waves in a patient with WPW is variable — most leads in Figure-1 do not seem to have delta waves.
- Finally, looking closer — it may be that delta waves are simulated (and not present) in leads V1 and V3 because the initial part of the QRS lies near the baseline.
Bottom Line:
- Failure to consider WPW (especially in the presence of monophasic QRS widening in lead V1 with uncertain atrial activity, and uncertain PR interval) — will result in overlooking WPW when it does occur.
- Acutely, in this 60s woman with new CP — regardless of whether or not WPW is present, prompt cath is indicated because of the extreme ST-T wave changes in multiple leads that would be abnormal even if WPW was present.
- There is time to determine if today’s patient has WPW (ie, Review of this patient’s previous medical history and prior ECGs should be enlightening). In contrast — the decision to perform prompt cath is time dependent. Fortunately, this patient’s providers immediately recognized the acute ECG findings and expedited cardiac cath — that confirmed proximal total LAD occlusion, which was successfully stented.