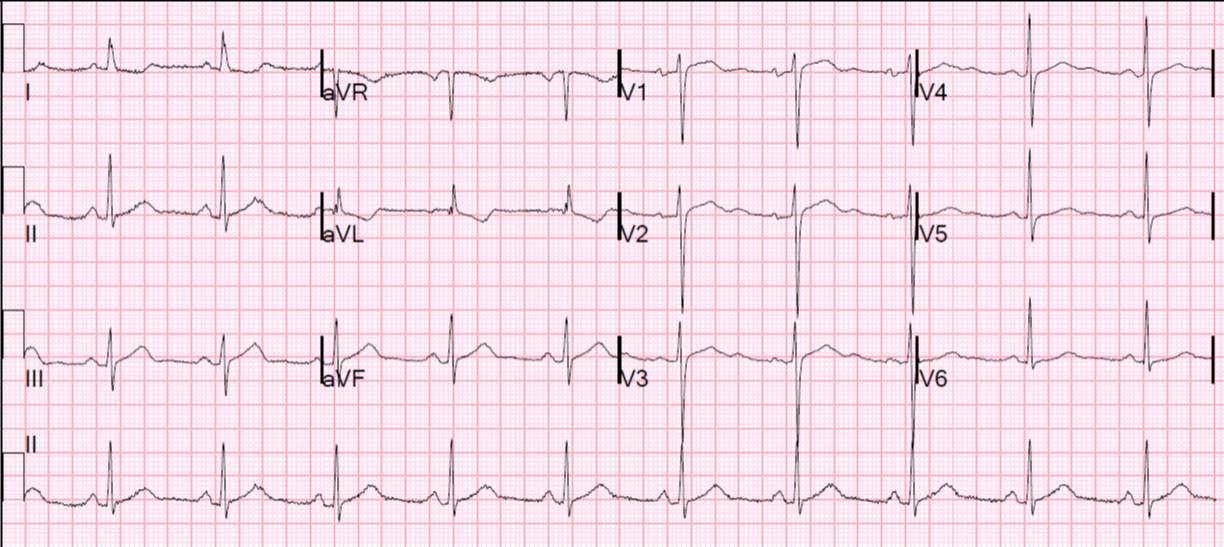
A middle-aged woman with a history of hypertension presented with typical chest pain. Her BP was 160/80. Here was her presenting ECG, with chest pain:
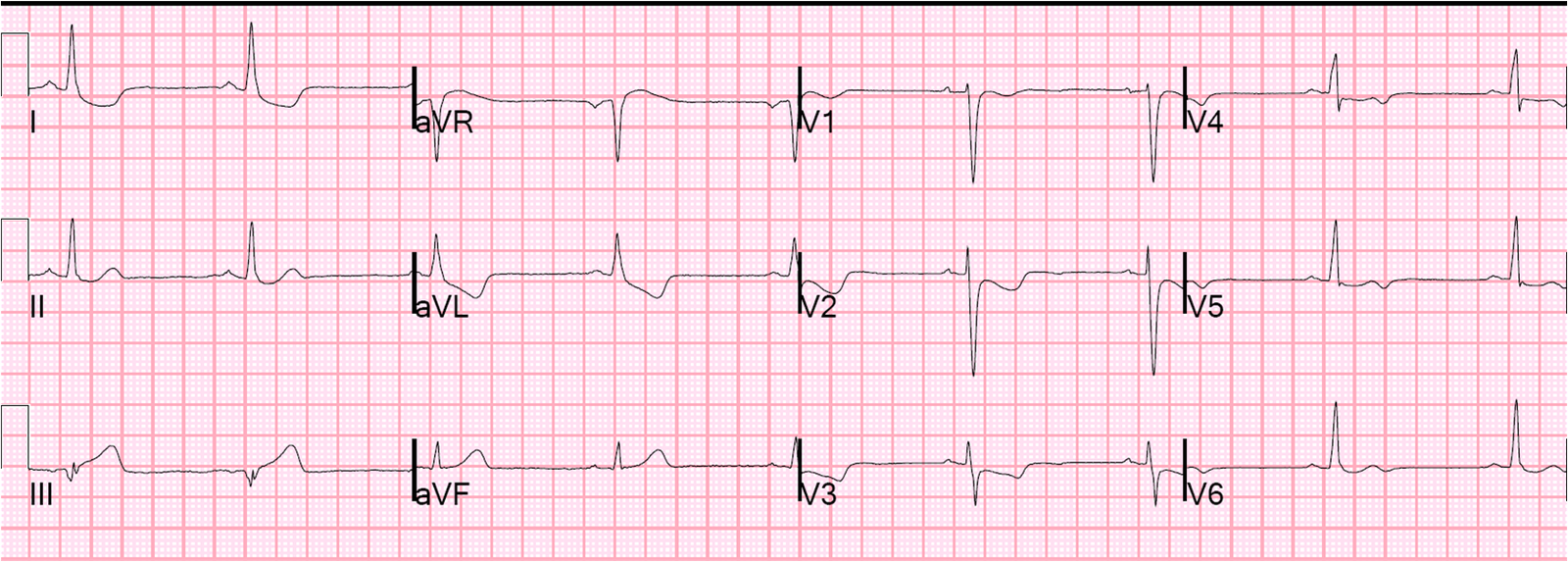
The pain improved with Nitroglycerine. Creatinine was 4.3. She underwent another ECG at 6 hours (when she was pain free):
The troponin peaked at 16 ng/mL (also retrospectively diagnostic of OMI) and there was a “probable” inferior wall motion abnormality.
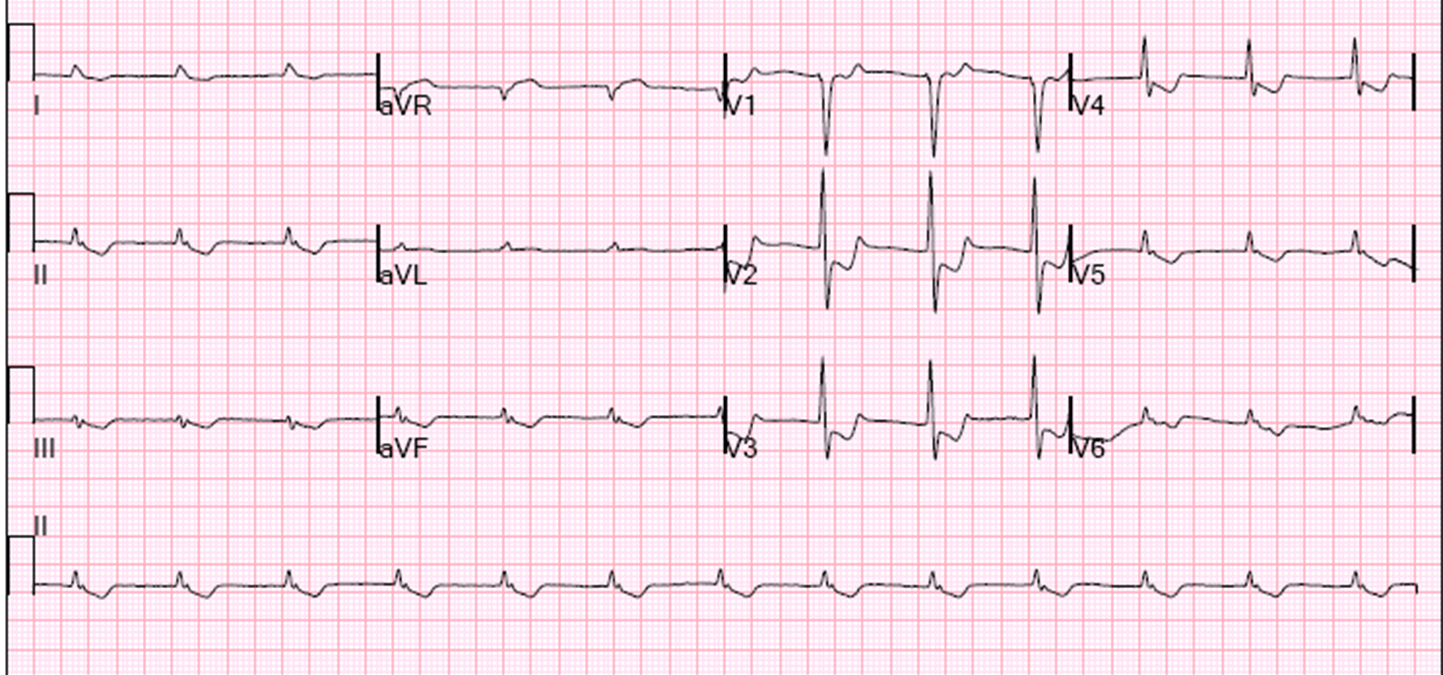
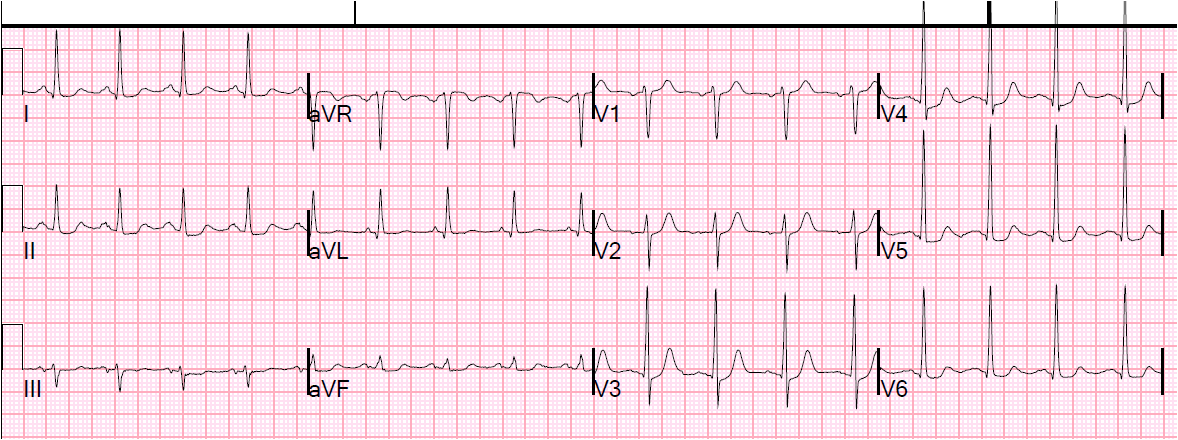
Because the patient had advanced renal insufficiency and because there was “no evidence for a current of injury on her presenting EKG’s”, a non-invasive approach was undertaken. While undergoing a stress test as a part of the non-invasive approach, she developed chest pain and hypotension and had this ECG:
She went immediately to angiogram and had occlusion of the RCA at the ostium.
Looking back, one can see ST elevation in V1-V3 on the initial ECG that is nonspecific, but, in retrospect, is probably due to RV Injury.