A male in his mid 30s with no cardiac history but some cardiac risk factors had onset of chest pain and arrived in the ED within 30 minutes of onset.
He was brought directly to a room, where our Hennepin ED ultrasound guru Dr. Robert Reardon performed a bedside cardiac ultrasound immediately, before an ECG could be recorded.
Drs. Reardon and Scott Joing of Hennepin are Editors of Ma and Mateer’s Ultrasound Textbook and, along with Andrew Laudenbach (also of Hennepin), authors of its cardiac ultrasound chapter.
Here is the initial parasternal short axis echo:
Dr. Reardon read this as an inferior wall motion abnormality. The most obvious finding to me is the asymmetry of contraction
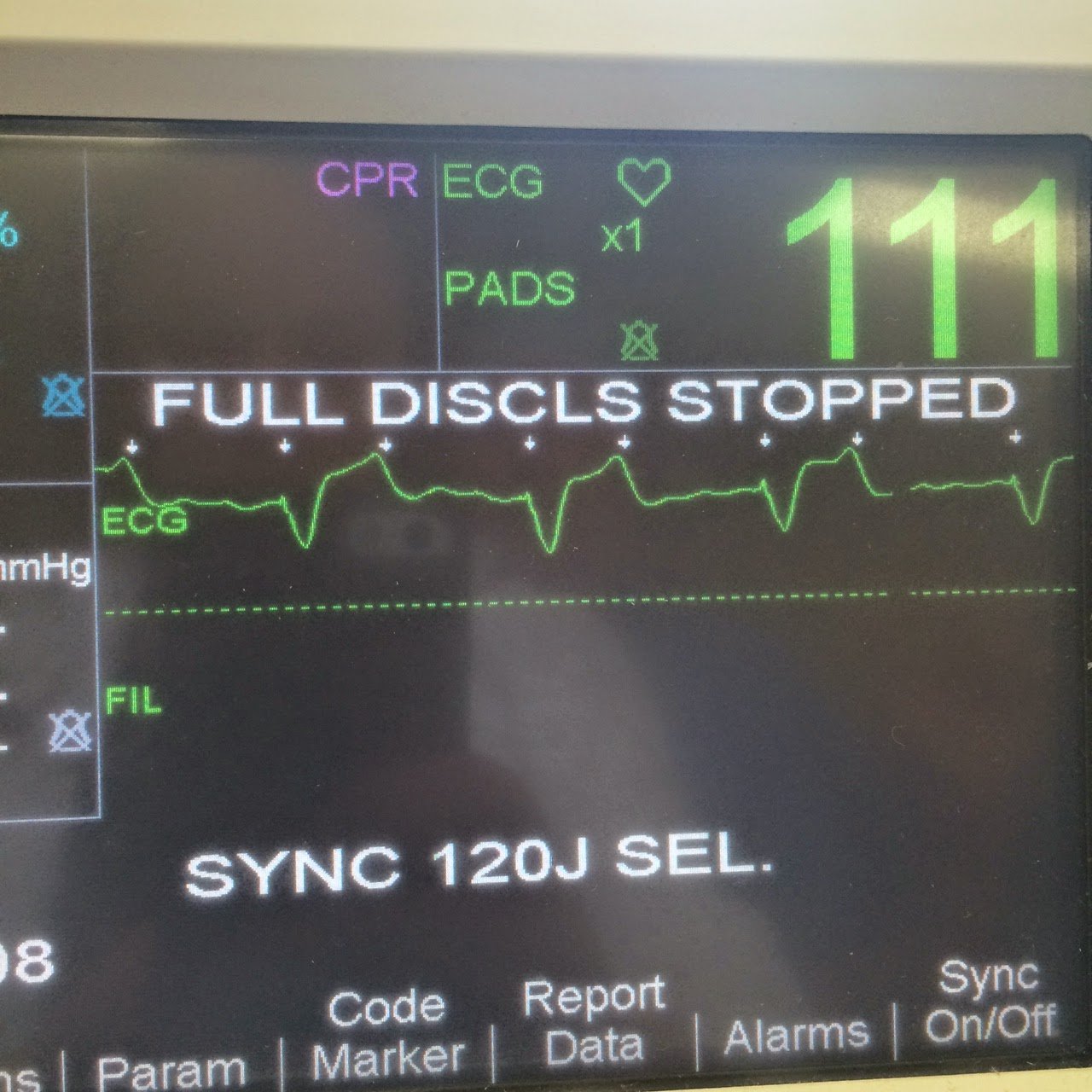
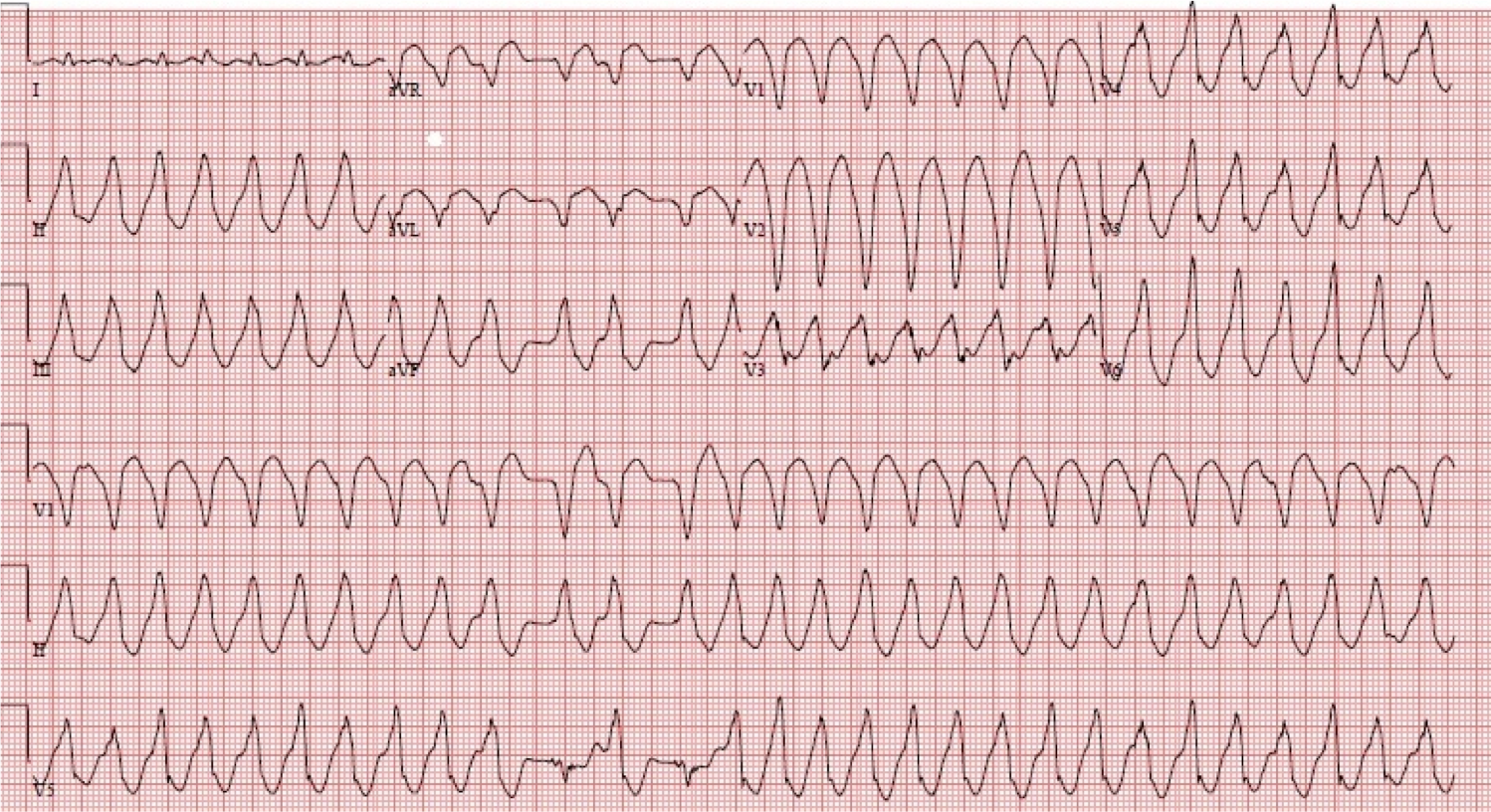
An ECG was immediately recorded. I was there with Dr. Reardon to read it. Its findings are (to me) much more obvious:
A right sided ECG was recorded:
 |
| V1-V6 are really V1R – V6R. There is clearly greater than 0.5 mm of ST elevation in V4R.
This is nearly diagnostic of Right Ventricular injury |
His blood pressure was good and there was no evidence of RV infarct physiology.
The patients pain was unrelenting. The diagnosis was clear. The cath lab was activated in the middle of the night just minutes after the patient arrived.
Dr. Reardon proceeded to record some images using “Speckle Tracking,” in which, after telling the computer where the endocardium is with a few markers, it automatically tracks wall motion of all the sectors, and even graphs their motion (on the right).
Here is a parasternal short axis:
5 of 6 segments contract, thicken, and shorten. The sixth (“inf”) on the lower left, does not do so. The graph at the right shows the degree of wall motion of each of the 6 segments. The top one, which has the least motion, is the line representing that inferior segment.
Here is a second parasternal short axis:
Here is a still frame:
|
Here is an apical 2 chamber view:
The segment on the lower left is the inferior wall, in purple, and you can see how it has no motion. On the graph, it is represented by the purple line at the top (it is at the top because it has so little wall motion)
|
Case continued
While waiting for the cath team, 2 more ECGs were recorded, with no evolution.
The patient was taken to the cath lab and had a 100% occlusion of the mid RCA. There were 4 Right ventricular marginal branches BEFORE the occlusion. So the right sided ST elevation is unexplained.
Also, there were good left to right collaterals so that only a small portion of the inferior wall was completely ischemic.
This accounts for the subtle ECG findings and the lack of evolution.
The highest troponin I was 13 ng/mL.
Here is the post cath ECG:
 |
| All ST elevation is resolved. There are subtle inferior Q-waves of infarction. |
6 hours later, another ECG was recorded:
 |
| Now there is T-wave inversion in III, with well formed pathologic Q-waves of infarction. |