Case 1.
A woman in her 60s with no prior history of CAD presented with 3 hours of sharp, centrally located chest pain with radiation to the anterior neck, with associated nausea. She had known HTN and DM. She appeared to be in distress. She was given sublingual NTG with improvement, but there was not complete resolution.
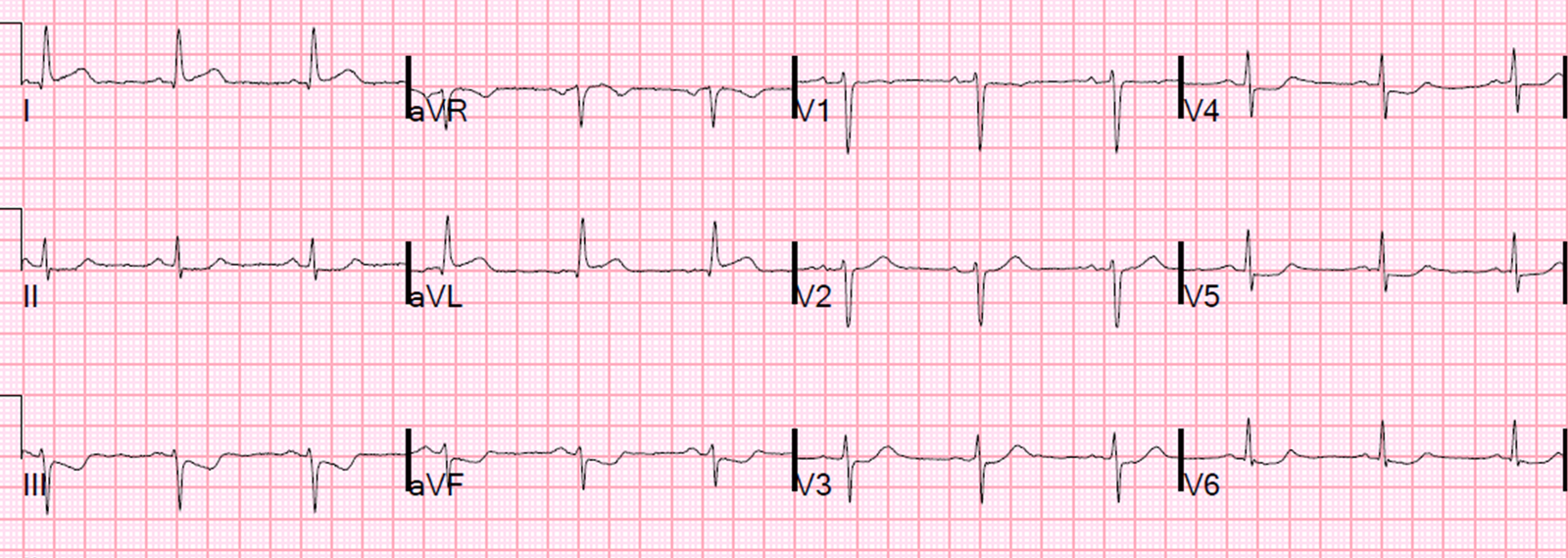
Here was here initial ECG:
It is important to compare this one with the false positive case #3 at the bottom; that one is a case which could fool you.
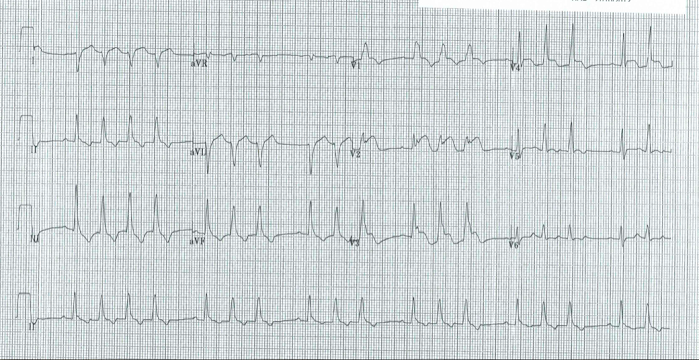
There was an old ECG for comparison:
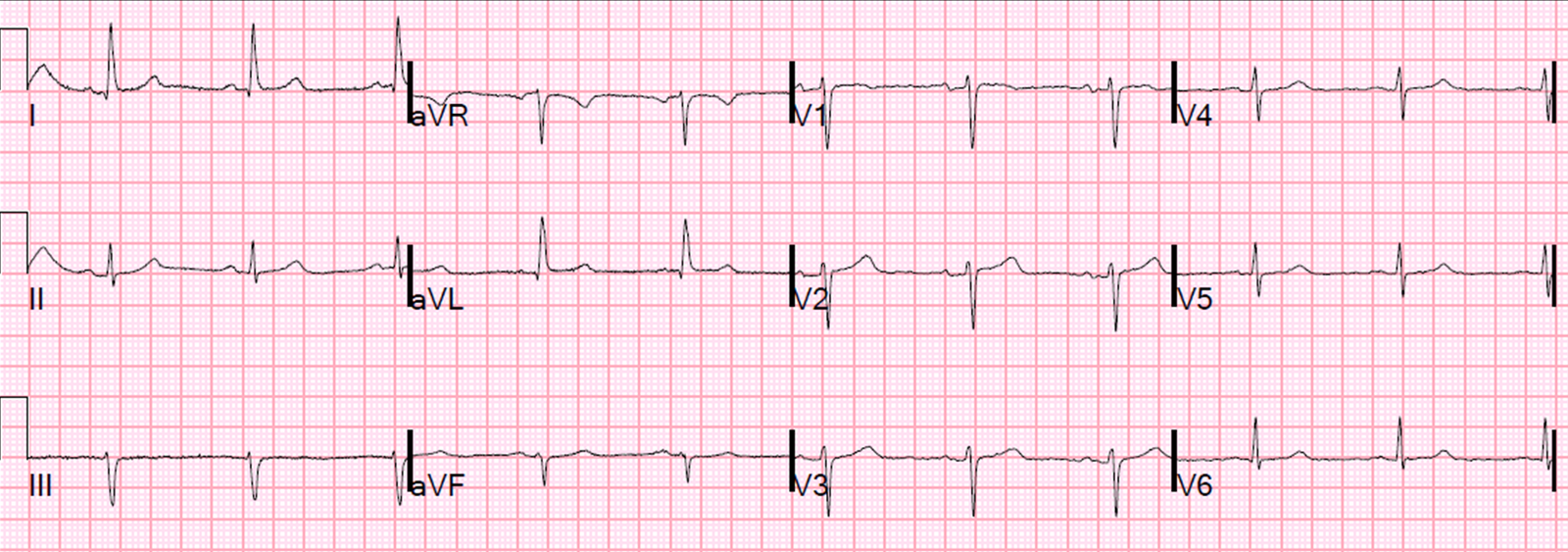 |
| One year prior with no ST segment abnormalities |
A bedside cardiac ultrasound was done by the emergency physician. Here is the parasternal short axis view:
There is an anterior and lateral wall motion abnormality.
This still helps to show the wall motion abnormality:
 |
| Arrows point to area of wall motion abnormality |
The Cath Lab was activated, and here are the results:
1. LM: No significant stenosis.
2. LAD: luminal irregularities with a 40% stenosis at the take-off of a D3. D3 has a 95% tubular ostial stenosis. (Culprit, stented)
3. LCX: Luminal irregularities, no significant stenosis. Two OM branches without significant stenosis.
4. RCA: dominant. Luminal irregularities without significant stenosis. Supplies a small RPDA and RPLA.
After cath lab activation, her initial troponin returned at 0.124 ng/mL (99% level = 0.030 ng/mL)
This was the post-cath ECG:
 |
| After reperfusion: aVL shows resolution of ST elevation and inverted (reperfusion) T-wave. There is also some terminal T-wave inversion in anterior precordial leads |
A large Diagonal artery may supply both the lateral wall and part of the anterior wall.
Case 2: Another subtle lateral MI, from this post:
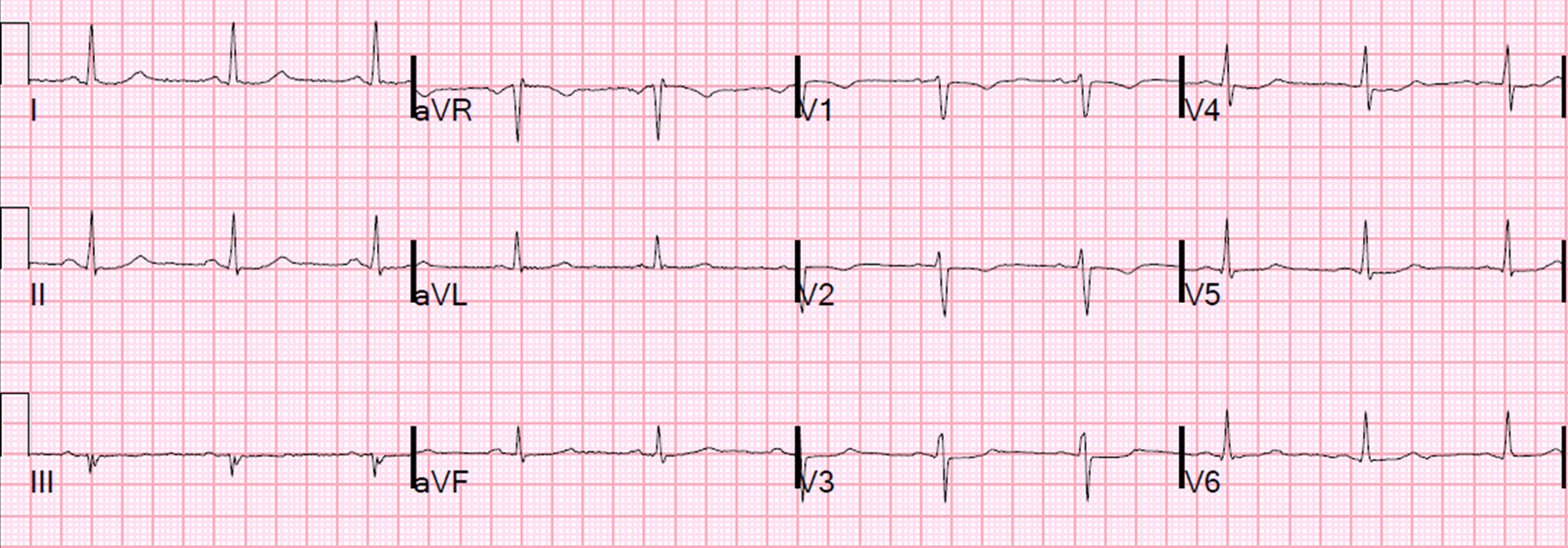
A male in his 60’s presented 30 minutes after the onset of crushing substernal chest pain. Medics recorded 2 ECGs, one before and one after sublingual NTG, and both are similar to the first ED ECG. The patient had never had pain like this before. The pain improved from 9/10 to 3/10 after NTG. Here is the initial ED ECG:
This ECG, especially along with the very typical
history, was very worrisome, but not absolutely diagnostic of, ischemia.
Several serial ECGs showed no change, even after the pain finally resolved to
0/10 after NTG.
He was given aspirin, clopidogrel, IV nitroglycerine,
and heparin, the general cardiologist was called and notified that this patient
was very high risk and needed close attention. He readily agreed, and the
plan was to admit for close observation, serial ECGs and troponins, and to
scrutinize for any recurrence of pain or change in the ECG.
The first troponin I then returned at 0.063 ng/ml
(upper limit of normal = 0.025 ng/ml).
Repeat ECG remained unchanged.
–He remained pain free and the plan remained to admit with a diagnosis of
Non-STEMI on medical therapy with plan for angiogram in the
morning.
–Just before admission to the hospital, the patient admitted to recurrent pain
and appeared uncomfortable. Therefore, the cath lab was activated urgently.
–The suspicion was for a circumflex (or obtuse marginal branch) or diagonal
artery occlusion or subtotal occlusion.
–At cath, there was a 95%
proximal LAD stenosis with TIMI-II flow, proximal to a large
diagonal. A stent was placed and the patient became pain free.
Case 3: False positive
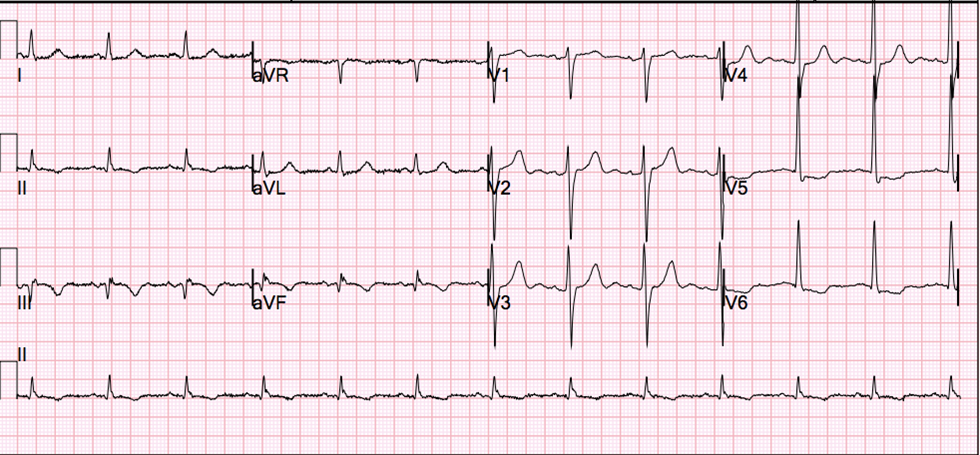
And here is a similar one that is NOT MI. How do we tell the difference?
 |
| There is ST elevation in I and aVL, with reciprocal ST depression in lead III. |
Just so you don’t think I’m cheating by using a retrospectoscope, this was sent to me without any outcome, and I read it as “no MI” with a high degree of certainty. This is because:
1. The remainder of the ECG is normal. No poor R-wave progression, no other ST depression, no symmetrical T-waves, no large T-waves, no down-up T-waves, typical early repol in anterior leads
2. The reciprocal ST depression is in lead III only. Not in leads II and aVF.
3. There are distinct J-waves in the two leads with ST elevation. This is highly suggestive of early repolarization in these leads.
4. The T-waves in I and aVL are not large (this was also true with the MI case 1 at the top, but that case had many other suspicious findings (many leads with ST depression and no J-waves)
Lessons:
When there is ST elevation in aVL, with reciprocal ST depression in III:
1. Look for:
a. J-waves
b. Other ST depression
c. Large T-waves
d. Symmetric T-waves
e. Down-Up T-waves
2. Compare with an old ECG
3. Use ED Echo if available
4. Use formal Echo
5. A positive troponin is helpful (a negative one is not)