This patient called 911 for chest pain. The medics did an amazing job of recording serial ECGs.
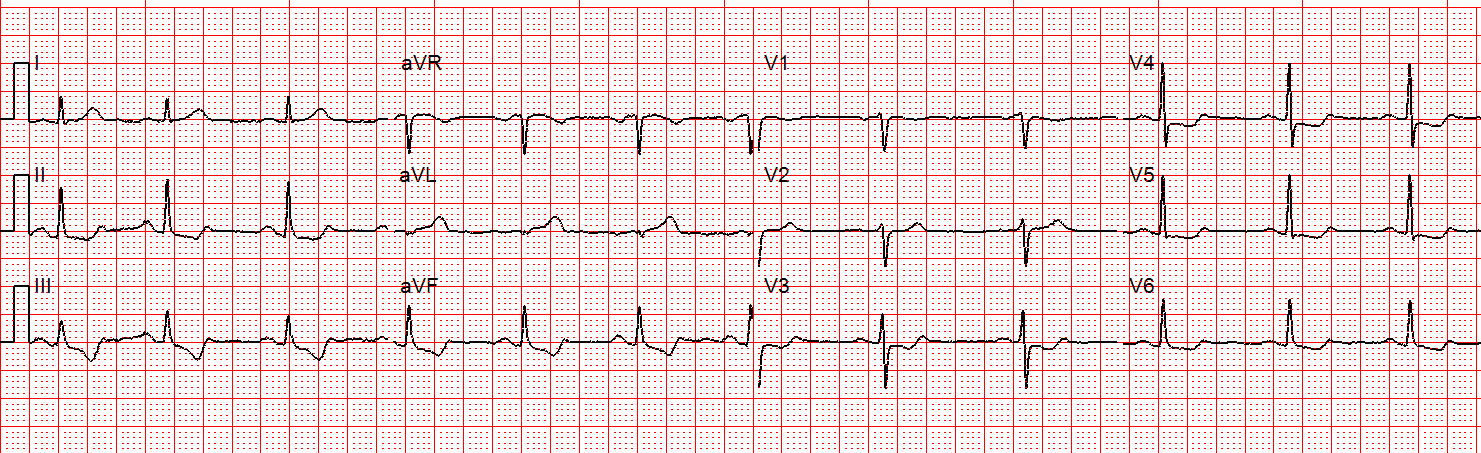
Time zero
1 minute
 |
| Not much change |
3 minutes
 |
| Still not much change |
5 minutes
 |
| Slightly less ST depression Is the subendocardial ischemia diminishing? |
14 minutes
 |
| Significantly less precordial ST depression More inferior ST depression |
17 minutes
Midanterolateral MI:
STEMI: Which coronary artery is occluded?
Is this acute coronary occlusion? Simple ACS? Where is the culprit lesion?
Recordings continue
19 minutes
23 minutes
 |
| About the same |
24 minutes
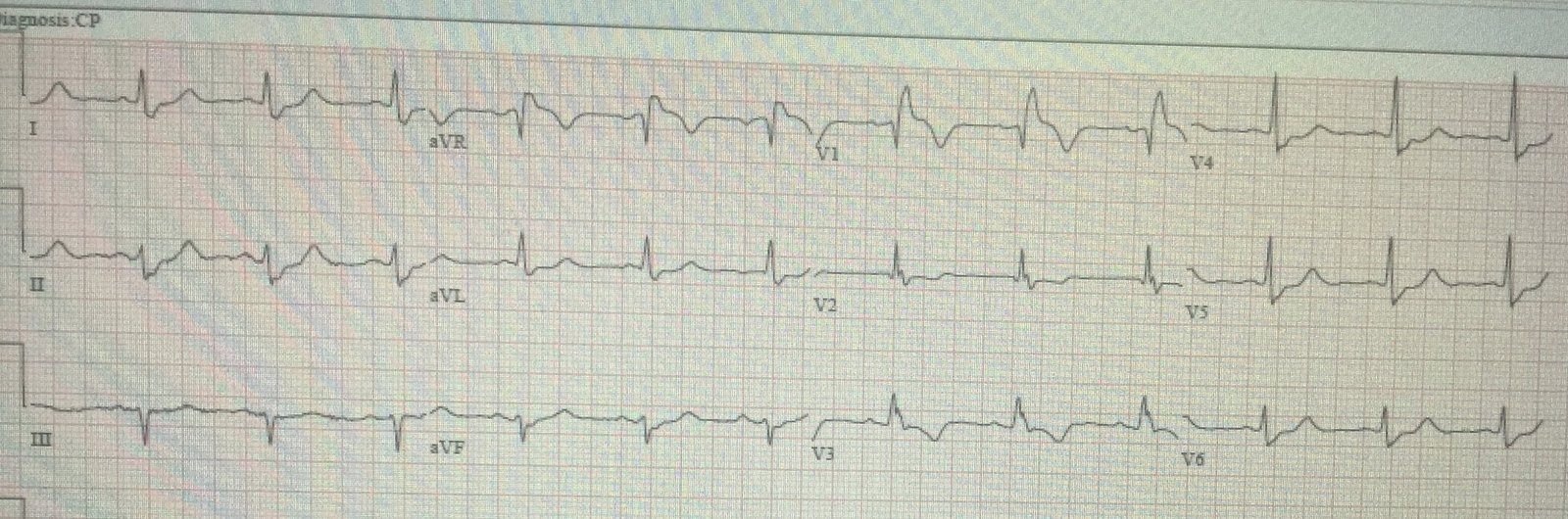
 |
| More ST Elevation/Depression |
26 minutes
The patient was taken to the cath lab.
A proximal thrombotic LAD occlusion was found. There was no detail about whether it was directly at the ostium of the first diagonal or not.
==================================
Comment by KEN GRAUER, MD (11/15/2018):
==================================
It’s hard to imagine a better post than this one for the recording of serial ECGs to illustrate the evolution of an extensive acute STEMI. I focus my comments on some additional teaching points to the excellent discussion by Dr. Smith.
- For clarity and ease of comparison — I’ve selected just 4 of the 10 tracings to highlight important serial changes (Figure-1).
==========================
ECG #1: ( = the Initial Tracing @ Time = Zero):
As per Dr. Smith — the KEY to assessment of ECG #1 lies with the appearance of the ST-T wave in lead aVL. That’s because without lead aVL — the picture would essentially be that of diffuse ST-T wave depression, with slight ST elevation in lead aVR. In a patient with new chest pain — this would suggest probably significant coronary disease — but not acute occlusion!
- Adding lead aVL to this picture in ECG #1 adds urgency to the situation. Despite no more than subtle ST elevation in aVL — the disproportionately tall, peaked and fatter-than-they-should-be T wave in lead aVL clearly suggests that this is an acute change.
- Confirmation that what we see in lead aVL is acute — is forthcoming from the mirror-image opposite picture of the ST-T wave in lead III. In association with similar-looking (though not quite as marked) ST-T wave depression in the other 2 inferior leads (leads II and aVF) in this patient with new chest pain — there should no longer be any doubt that the hyperacute appearance in lead aVL of ECG #1 is real.
 |
| Figure-1: Comparison between 4 of the 10 serial ECGs recorded in this case (See text). |
==========================
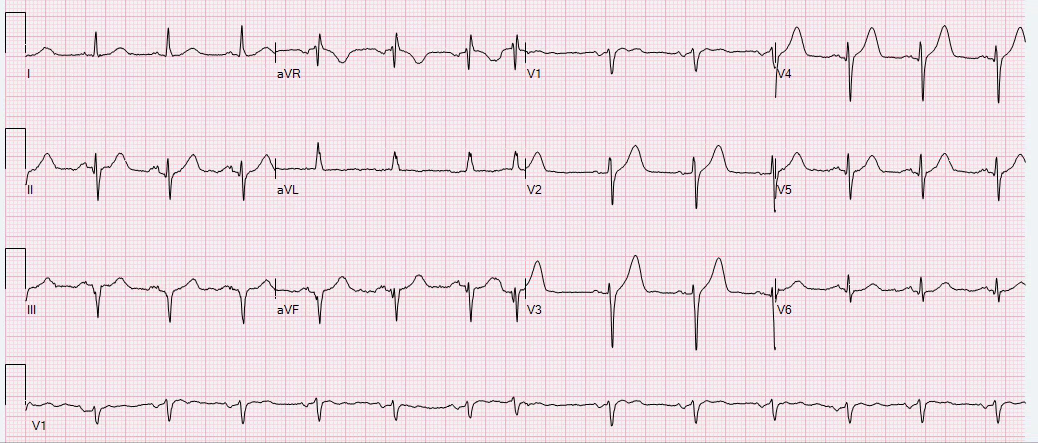
Question A — Why is there is less ST depression in the chest leads for ECGs #5 and #6 — compared to the amount of ST depression seen in the chest leads for initial tracing ECG #1?
- HINT — Be sure to review ECG #8 before answering.
================
Answer — If one simply looked at the 6 chest leads in ECG #5 alone — one would never guess this patient was in process of evolving an extensive anterior STEMI. That’s because the ST-T waves in the chest leads of #5 offer a transition look between more prominent chest lead ST depression in ECG #1 — and, progressive T wave peaking, leading to frank chest lead ST elevation in ECGs #6 and 8.
- MORAL — If you happen to “catch” the patient at a moment in between evolution from ST depression on-the-way-to ST elevation — the temporary result might be minimal ST segment deviation. That’s why serial tracings are needed.
==========================
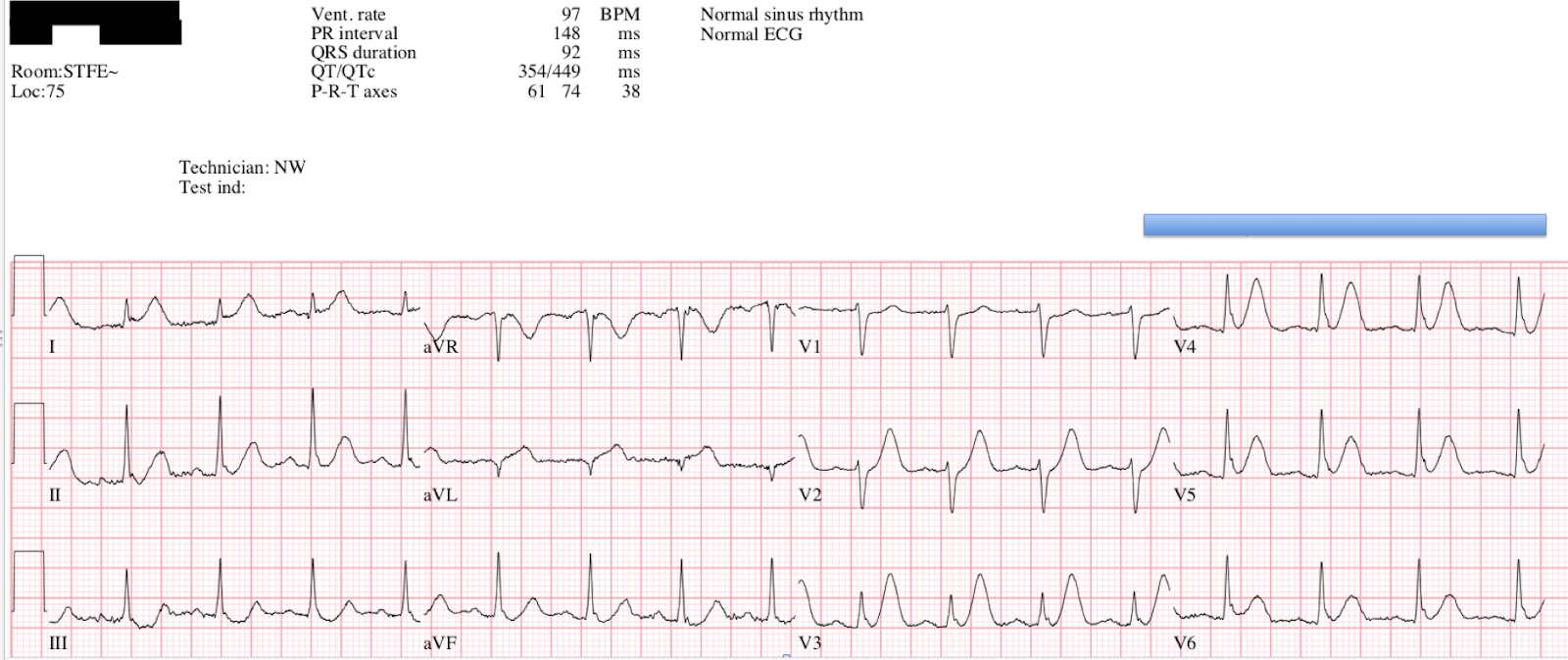
Question B — What happens to the frontal plane axis during the course of 23 minutes as one follows the sequence of ECG changes from ECG #1 until ECG #8?
================
Answer — The frontal plane axis progressively shifts to the left as one follows serial tracings, especially from ECG #5 until ECG # 8.
- Note development of an S wave in leads III and aVF in ECG #6.
- S waves deepen, and the QRS complex becomes predominantly negative in all 3 inferior leads by the time ECG #8 is recorded. This is consistent with a frontal plane axis more negative than -30 degrees — which satisfies criteria for LAHB (Left Anterior HemiBlock).
- Support that this leftward axis shift truly indicates development of a new conduction defect is forthcoming from the ~0.02msec of additional QRS widening now evident in ECG #8.
- NOTE — New hemiblock is another indicator of the extent and severity of this acute STEMI.
==========================
Question C — Going back to ECG #1, what findings in this initial ECG should alert us that this picture might soon evolve to the anterior STEMI seen in ECG #8?
================
Answer — As emphasized by Dr. Smith — the hyperacute ST-T wave in lead aVL of this patient with new chest pain suggests possible LCx (Left Circumflex), 1st or 2nd Diagonal branch, or LAD (Left Anterior Descending) occlusion in ECG #1 — depending on what other leads on the ECG will evolve to show.
- Dr. Smith highlighted the finding of ST depression in multiple leads in ECG #1 — which suggested diffuse subendocardial ischemia. In this context — I would not have expected to see a straight, isoelectric ST segment with a clearly upright T wave in lead V2 unless the picture in ECG #1 was about to transition to ST segment elevation in this V2 lead. While impossible at this point to be certain of what was soon to come — lead V2 was clearly a lead to watch!
==========================
BOTTOM LINE —There is MUCH to be learned from careful review of serial tracings. Retrospective self-analysis after all the ECGs in a case have been recorded and the end-result is known — is perhaps the best way to hone our skills for prospectively recognizing changes the next time a similar case is encountered.
- SUGGESTION — It may be worthwhile to spend a final moment revisiting the serial changes in each of the leads for the 4 ECGs sequentially shown in Figure-1.